Prioritizing Patient Health in Texas & the US by Integrating the Non-Medical Drivers of Health

Table of Contents
Author(s)
Elena M. Marks
Senior Fellow in Health PolicyJacquie Klotz
Program Manager, Center for Health and BiosciencesRebecca Mak
Graduate Student, Harvard's TH Chan School of Public HealthShare this Publication
- Print This Publication
- Cite This Publication Copy Citation
Elena M. Marks, Jacqueline Klotz, and Rebecca Mak, "Prioritizing Patient Health in the US & Texas by Integrating Non-Medical Drivers of Health into the Health Care System" (Houston: Rice University’s Baker Institute for Public Policy, June 8, 2023), https://doi.org/10.25613/ky97-1j38.
Introduction
The United States spends far more on health than other high-income countries, whether measured by total dollars expended, per capita spending, or share of gross domestic product (GDP). Health expenditures in the U.S. have escalated dramatically over the last 40 years, rising from $253 billion or 8.9% of GDP in 1980 to $4.3 trillion or 18.3% of GDP in 2021. If the U.S. were achieving the full value of this investment, we would expect to see it ranking high by health outcomes, but instead, the U.S. underperforms compared to other high-income countries. The U.S. has the highest rates of infant and maternal mortality among comparable countries, and its life expectancy falls below the OECD average. In fact, the gap in health expenditure and life expectancy between the U.S. and other high-income countries has grown dramatically over the last 40 years, as shown in Figure 1. While U.S. medical care is perceived as cutting-edge, equipped with the latest technology, and with an ever-growing sector for pharmaceutical drugs and devices, we lag far behind other countries in some of the most basic indicators of national health.
Figure 1 — Life Expectancy and Health Care Spending Per Capita, 1980-2021
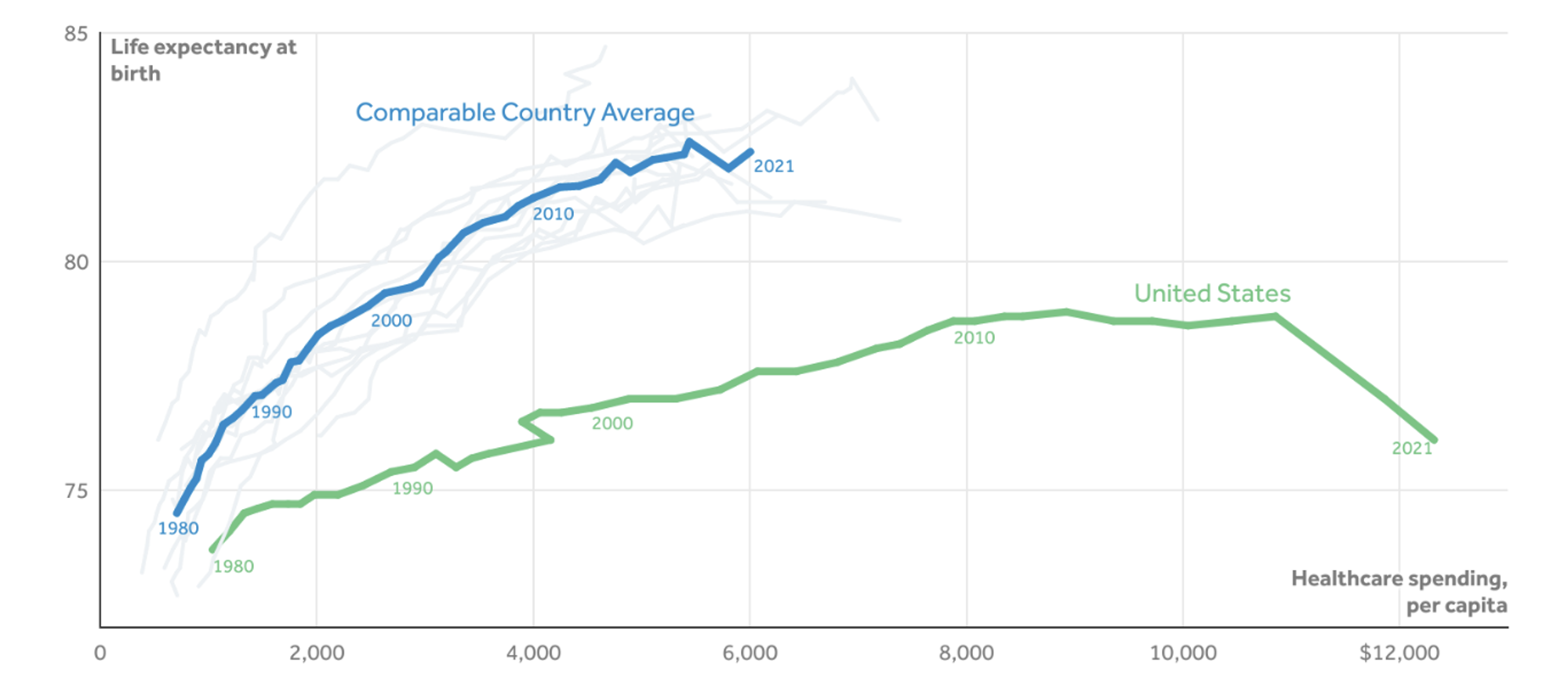
Source Peterson-KFF Health System Tracker: KFF analysis of CDC, OECD, Japanese Ministry of Health, Labour, and Welfare, Australian Bureau of Statistics, and UK Office for Health Improvement and Disparities data.
Non-Medical Drivers of Health are Key to Health Outcomes
The National Academy of Medicine has long acknowledged that medical care addresses only 10%-20% of the factors that drive health outcomes, while social, environmental, economic, and behavioral factors drive 80% of outcomes. In recognition of this, the health care system has begun to include non-medical interventions in delivery and payment systems. Known in the literature as social determinants of health (SDOH), and referred to in Texas and in this brief as non-medical drivers of health (NMDOH), these factors are defined as “the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life.” A growing body of evidence demonstrates that for some populations, non-medical interventions that address housing, nutrition, transportation, and other social drivers can improve health outcomes and, in some cases, reduce medical care costs. Incorporating services that address unmet NMDOH needs within the health care system represents an emerging opportunity to improve population health outcomes to deliver greater value for U.S. health spending.
Health insurance plans, community clinics, hospital systems, and other providers are well-positioned to ensure their patients have access to resources to address unmet NMDOH needs. This work is already underway across the United States. Familiar examples include food assistance programs ranging from routine food insecurity screenings to weekly grocery deliveries for patients via local food pantry partnerships and even the delivery of medically-tailored meals. Other examples are home remediation programs, which remove asthma triggers in the home and reduce the asthma attacks that lead to emergency room visits. Hospital-driven housing initiatives are yet another example that connect chronically homeless patients who frequently visit emergency departments to permanent supportive housing.
While this work is promising, and the evidence base is growing, these programs face challenges reaching all patients in need because of funding limitations that impede scaling and sustainability. This issue brief outlines notable new policies at the national and state levels that support sustainable funding for addressing unmet NMDOH needs and improving health outcomes.
National Action
Health Insurance Rating System to Include NMDOH Measures
Public and private purchasers of group and individual health insurance plans look at performance measures to compare quality among plans and select the best plan for their needs. To support plan comparison, the National Committee for Quality Assurance developed the Healthcare Effectiveness Data and Information Set (HEDIS) to track the performance of plans. HEDIS data is used to monitor and compare health plan quality and performance, and identify areas for improvement. Covering more than 90 health care dimensions, from immunization status to well-care visits to management of chronic conditions, HEDIS measures indicate how well plans are delivering health to their enrollees. Because over 200 million Americans are covered by health plans that use HEDIS, the measures on which they collect data influence health plan and provider behavior.
HEDIS often uses process indicators as proxies for patient health outcomes. For example, HEDIS counts the number of well-child visits in the first 30 months of life as a proxy for child health. This measure assumes that if the visits occur, a child will be healthier. While the occurrence of a visit is an easy and valuable metric, it fails to capture the impact of the visit on the child’s health. Is the child truly healthier because they visited the provider?
Social Need Screening and Intervention
HEDIS continuously refines its measurements to better reflect health outcomes. In 2023, HEDIS added the Social Need Screening and Intervention (SNS-E) measure that signifies a shift toward metrics that measure patient health outcomes and recognizes the importance of addressing non-medical needs as an indication of health care quality.
The SNS-E captures both screening for unmet non-medical needs — a traditional process measure — as well as an intervention component to indicate whether the patient actually received an appropriate and timely intervention for their unmet non-medical need. For 2023, the SNS-E will measure unmet needs relating to food, housing, and transportation. While many providers have integrated screening into their health care delivery, consistent connection of patients with the services to address their non-medical needs does not always occur. The inclusion of the SNS-E as a quality indicator is expected to incentivize health plans, which will then incentivize their providers, to ensure patients receive resources for unmet non-medical needs, thus supporting a delivery of care that achieves better patient health outcomes.
Funding NMDOH through Medicaid In Lieu of Services or Settings
Medicaid offers another new opportunity to accelerate the inclusion of non-medical drivers into the health care delivery and financing system. Medicaid is a public health insurance program, funded by the federal and state governments, for low-income people and those with disabilities. In 2022, 85 million Americans, including 5 million Texans, received their health insurance through Medicaid. Medicaid is regulated by the Centers for Medicare and Medicaid Services (CMS) and administered through state Medicaid offices. The design of the Medicaid program influences how plans and providers are paid for the provision of health services.
In January 2023, CMS provided new guidance to state Medicaid directors outlining a mechanism for Medicaid to pay for non-medical services that improve Medicaid enrollee health outcomes by using a provision called In Lieu of Service or Setting (ILOS). The guidance requires that non-medical services must be 1) medically appropriate and cost effective, 2) optional for enrollees, 3) authorized and specified in the managed care plan contract, and 4) considered in setting capitation rates for services included in state health plans. For example, according to these guidelines, ILOS can be applied to medically tailored meals for populations suffering from chronic conditions that can be improved with proper nutrition. The ILOS guidance exemplifies CMS’ recognition of the benefit of NMDOH services in improving patient health outcomes, and that patient outcomes should be the key driver of health care spending. In turn, Medicaid providers can focus on giving patients what they need to be healthier, rather than restricting care to medical services.
Similar to the SNS-E metric, the ILOS guidance is a prioritization of patient health outcomes, rather than the delivery of discrete medical services, as the purpose of health care.
Texas Action
Momentum toward the integration of non-medical services into the health care system is growing in Texas. Health plans, hospital systems, and other providers have established programs targeting NMDOH and continue to pursue sustainable funding for these services. Texas is acting to match national efforts through agency and legislative action.
HHSC Medicaid & CHIP Services NMDOH Action Plan
The Texas Health and Human Services Commission (HHSC) has formally recognized the impact of NMDOH services as well as the delay in Texas state-funded pathways for payment for services that address unmet NMDOH. In February 2023, HHSC released a Medicaid & CHIP Services NMDOH Action Plan, outlining a strategy to address NMDOH needs for Medicaid enrollees in Texas. With a focus on food insecurity, housing, and transportation, the plan lays out steps to integrate NMDOH services into the health care system and its payment structure over the next four years.
- First, the plan calls for measuring and evaluating existing NMDOH programs in Texas Medicaid.
- Next, HHSC will design and implement payment strategies to incentivize providers and managed care organizations to screen and provide interventions for unmet NMDOH needs using strategies including ILOS, value-based payment models, and other quality measures.
- Finally, HHSC plans to facilitate working groups with stakeholders throughout Texas and at the federal level to disseminate best practices and form effective partnerships with NMDOH service providers. These working groups will include Medicaid beneficiaries to capture the needs and perspectives of intended recipients.
The goal of the action plan is to improve population health and cut preventable downstream medical spending in Texas. In the first year, HHSC will focus on unmet food needs and will build an infrastructure to support the plan, extending to housing and transportation over the next three years. Since the plan was released in February 2023, key health care stakeholders have shared their enthusiasm and provided feedback to align on next steps in Texas. HHSC’s recognition of the significance of NMDOH, as well as this plan’s acknowledgement of the state as a funder of NMDOH screening and service delivery, indicates the early stages of a health spending transformation in Texas.
2023 Legislation
For the first time in June 2023, Texas enacted a law that recognizes the importance of non-medical drivers of health. During the recently completed legislative session, HB 1575 was enacted: It enables Texas Medicaid to improve health outcomes for pregnant women by paying for non-medical case management services offered by, among others, community health workers and doulas. The act specifically recognizes the impact of non-medical factors on health outcomes as its basis. The legislation provides direction to the state Medicaid agency to screen for non-medical health-related needs and to pay for case management to help qualified patients obtain non-medical services such as nutrition and housing supports, parenting services, and domestic violence assistance. The agency is directed to establish provider reimbursement categories for community health workers and doulas so these non-medical health professionals can be paid for their work.
Also during this session, the legislature in HB 12 expanded post-partum Medicaid coverage to 12 months (from two), which means women can benefit from these new services for a full year after delivery. This will benefit many Texas families as over 180,000 births in Texas were covered by Medicaid in 2021.
Texas Consortium for the Non-Medical Drivers of Health
An organized field of practice is emerging for those working in the NMDOH space in Texas. To advance the research, policy, and practice of NMDOH in Texas, Rice University’s Baker Institute for Public Policy and UT Health School of Public Health’s Center for Health Care Data founded the Texas Consortium for the Non-Medical Drivers of Health (Texas Consortium). The Texas Consortium convenes researchers, practitioners, and policymakers to encourage the exchange of learning and knowledge in the NMDOH area and build a field of practice. The Texas Consortium began hosting learning sessions in June 2023 and will hold its inaugural conference on December 8, 2023. Public and private health plans, health systems, providers, academic institutions, and evaluators are participating in the consortium to build the field.
Conclusion
As we work to rein in escalating medical costs and improve health outcomes, the growing interest and investment in the non-medical drivers of health by the health care system in Texas and country-wide is promising. We look forward to continued momentum in this space at the federal and state levels.
This material may be quoted or reproduced without prior permission, provided appropriate credit is given to the author and Rice University’s Baker Institute for Public Policy. The views expressed herein are those of the individual author(s), and do not necessarily represent the views of Rice University’s Baker Institute for Public Policy.


