HRMS Issue Brief #15: The Impact of the Affordable Care Act on Texas Workers

Table of Contents
Author(s)
Vivian Ho
James A. Baker III Institute Chair in Health EconomicsElena M. Marks
Senior Fellow in Health PolicyPhilomene Balihe
Data Analyst, Episcopal Health FoundationShare this Publication
- Download PDF
- Print This Publication
- Cite This Publication Copy Citation
Ho, V., Marks, E., and Balihe, P. James A. Baker III Institute for Public Policy, Rice University, The Episcopal Health Foundation, Health Reform Monitoring Survey – Texas, Issue Brief #15: The Impact of the Affordable Care Act on Texas Workers.
In March 2015, near the close of the Affordable Care Act’s (ACA) Health Insurance Marketplace’s second open enrollment period, we surveyed adult Texans ages 18 to 64 to understand the changes in insurance status, if any, for Texas workers since the January 2014 effective date of many provisions of the ACA. Despite predictions that the ACA would erode Employer Sponsored Insurance (ESI), the data show that Texas workers experienced gains in ESI. In particular, lower income workers saw significant gains in ESI and in individually purchased plans. Lower income workers remain the largest group of uninsured working Texans and, despite the available subsidies in the Marketplace, the majority reported that they remain uninsured because the costs of coverage are too high.
About the Survey
The Health Reform Monitoring Survey (HRMS) is a quarterly survey of adults ages 18-64 that began in 2013. It is designed to provide timely information on implementation issues under the ACA and to document changes in health insurance coverage and related health outcomes. HRMS provides quarterly data on health insurance coverage, access, use of health care, health care affordability, and self-reported health status. The HRMS was developed by the Urban Institute, conducted by GfK, and jointly funded by the Robert Wood Johnson Foundation, the Ford Foundation, and the Urban Institute. Rice University’s Baker Institute and The Episcopal Health Foundation are partnering to fund and report on key factors about Texans obtained from an expanded, representative sample of Texas residents (HRMS-Texas). The analyses and conclusions based on HRMS-Texas are those of the authors and do not represent the view of the Urban Institute, the Robert Wood Johnson Foundation or the Ford Foundation. Information about the sample demographics of the cohort is available in Issue Brief #1. This Issue Brief is a summary of data extracted from the HRMS Survey in Texas that was administered in March 2015. We will continue to report on survey data through additional Issue Briefs and future surveys.
Changes in the Insurance Status of Texas Workers, 2013–2015
The ACA was designed to increase coverage among Americans by requiring large employers offer reasonably priced insurance to their workers (ESI) or pay a penalty and by creating a Marketplace where workers not covered by ESI could purchase affordably priced plans. The ACA encouraged workers to participate in ESI or purchase plans on their own by imposing an increasingly steep tax penalty for most who do not obtain coverage. From the outset, there were concerns that the Act would reduce ESI because employers would be incented to drop coverage. In this brief, “workers” include adult Texans ages 18-64 who are working for pay or are self-employed. “Lower income workers” are those with incomes at or below 250% of the federal poverty level ($50,000 for a family of three).
As Figure 1 shows, the percent of Texas workers covered by ESI actually increased from 2013 to 2015. This increase in ESI for all workers stands in stark contrast to the steady erosion of ESI across the country between 2000 and 2011. The Texas data are consistent with national data indicating stability in ESI since the implementation of the ACA.
Figure 1 — Texas Workers With ESI, 2013 and 2015
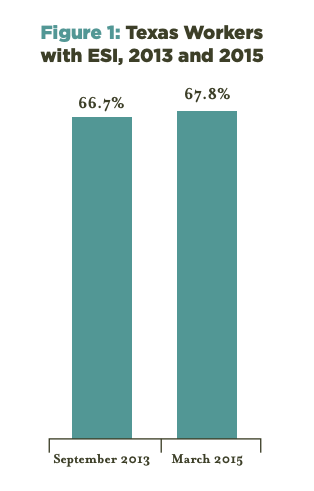
We also examined the changes in ESI from 2013 to 2015 for Texas workers based on income level. As we and others have reported, people with lower incomes are more likely to be uninsured than those with higher incomes. As Figure 2 shows, the increase in ESI among Texas workers is entirely attributable to those with lower incomes, experiencing a 12% increase in ESI while ESI coverage remained flat for those with higher incomes. The improvement in the rate of ESI for lower income workers may be attributable to increased employment in general, with large employers increasing offers of ESI to avoid paying a penalty for not providing affordable coverage, or lower income workers purchasing ESI they had previously refused to avoid paying a penalty for not obtaining coverage.
Figure 2 — Texas Workers With ESI by Income Level, 2013 and 2015
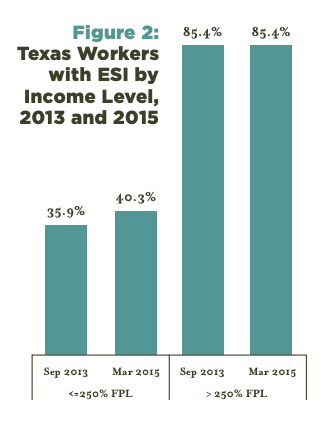
Access to Health Insurance for Lower Income Texas Workers, 2013–2015
Because lower income workers are more likely to be uninsured, we looked at the changes in insurance status and sources of coverage for those who were insured. Figure 3 below shows the percent of uninsured lower wage workers dropped by more than one-third, from 37.8% in 2013 to 24.4% in 2015. The 13.4 percentage point difference is attributable to a 4.4 percentage point increase in ESI and a 10.1 percentage point increase in individually purchased plans.
Notwithstanding the gains made by lower income workers from 2013 to 2015, this group’s rate of uninsurance is higher than the state average as reported by us in Issue Brief #11 and, more recently, by Gallup. When we asked survey respondents why they remained uninsured, the primary reason cited by more than half was that the cost is too high for them, as shown in Figure 4. This is consistent with other surveys including a recent report by The Commonwealth Fund. During 2014, we reported that the lowest monthly Marketplace premium, after subsidies, for a 30-year-old earning $23,340 annually was $50 per month, or $600 per year. This is currently higher than the tax penalty assessed for not having insurance. As the penalties increase, this population will have a greater incentive to purchase a plan.
Figure 3 — Insurance Status and Source for Lower Income Texas Workers, 2013 and 2015
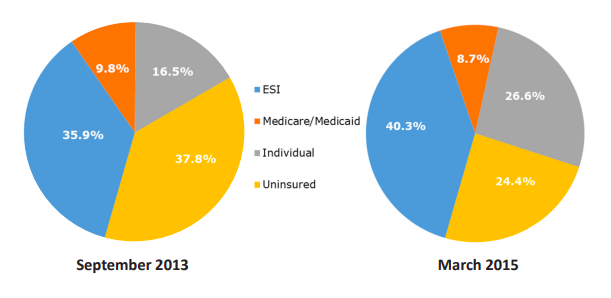
Figure 4 — Primary Reason Low Income Workers Remain Uninsured, March 2015
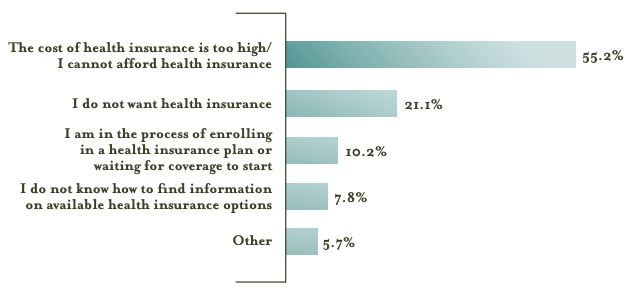
Looking Ahead
In our next brief, we will report on survey results from September 2015.
Methodology
Each quarter’s HRMS sample of nonelderly adults is drawn from active KnowledgePanel® members to be representative of the US population. In the first quarter of 2013, the HRMS provided an analysis sample of about 3,000 nonelderly (age 18–64) adults. After that, the HRMS sample was expanded to provide analysis samples of roughly 7,500 nonelderly adults, with oversamples added to better track low-income adults and adults in selected state groups based on (1) the potential for gains in insurance coverage in the state under the ACA (as estimated by the Urban Institute’s microsimulation model) and (2) states of specific interest to the HRMS funders.
Although fresh samples are drawn each quarter, the same individuals may be selected for different rounds of the survey. Because each panel member has a unique identifier, it is possible to control for the overlap in samples across quarters.
For surveys based on Internet panels, the overall response rate incorporates the survey completion rate as well as the rates of panel recruitment and panel participation over time. The American Association for Public Opinion Research (AAPOR) cumulative response rate for the HRMS is the product of the panel household recruitment rate, the panel household profile rate, and the HRMS completion rate—roughly 5 percent each quarter.
While low, this response rate does not necessarily imply inaccurate estimates; a survey with a low response rate can still be representative of the sample population, although the risk of nonresponse bias is, of course, higher.
All tabulations from the HRMS are based on weighted estimates. The HRMS weights reflect the probability of sample selection from the KnowledgePanel® and post-stratification to the characteristics of nonelderly adults and children in the United States based on benchmarks from the Current Population Survey and the Pew Hispanic Center Survey. Because the KnowledgePanel® collects in-depth information on panel members, the post-stratification weights can be based on a rich set of measures, including gender, age, race/ethnicity, education, household income, homeownership, Internet access, primary language (English/Spanish), residence in a metropolitan area, and region. Given the many potential sources of bias in survey data in general, and in data from Internet-based surveys in particular, the survey weights for the HRMS likely reduce, but do not eliminate, potential biases.
The September 2013 HRMS has a design effect of 1.47 for nonelderly adults, and a sampling margin of error for a 50 percent statistic with 95 percent confidence of +/- 1.3 for the nonelderly adult sample. The design effect for the Texas data in March 2015 is 2.184 and the MOE is +/- 3.7. The survey fielded from March 5-30.


