Check It: How Drug Testing Programs Can Reduce Overdose Deaths

Table of Contents
Author(s)
Share this Publication
- Print This Publication
- Cite This Publication Copy Citation
Katharine Neill Harris, "Check It: How Drug Testing Programs Can Reduce Overdose Deaths" (Houston: Rice University’s Baker Institute for Public Policy, September 2, 2022), https://doi.org/10.25613/4D6D-K841.
Every five minutes. That is, on average, how often someone in the U.S. dies from a drug overdose. The COVID-19 pandemic and the social disruptions it has caused have accelerated this crisis, now in its third decade. More than 100,000 Americans will fatally overdose in 2022, the second consecutive year with a death toll in the six figures.[1]
A complicated set of historical and structural factors explain why the U.S. holds the undesirable record for drug-related deaths among wealthy nations, but the most immediate problem today, easily identifiable, is the explosion of illicitly manufactured fentanyl on the unregulated drug market.[2] In 2011, fentanyl, a synthetic opioid 100 times stronger than morphine, was present in just 4% of overdoses; in 2021, 64% of fatal overdoses involved fentanyl or other synthetic opioids.[3] Fentanyl-related overdoses have surpassed car accidents as the leading cause of death for people 18-45.[4] Among adolescents, drug use rates are declining but overdose rates are increasing, with fentanyl present in 3 out of every 4 youth overdose fatalities in the first half of 2021.[5]
Figure 1 — Monthly Drug Overdose Deaths, January 2018–June 2021
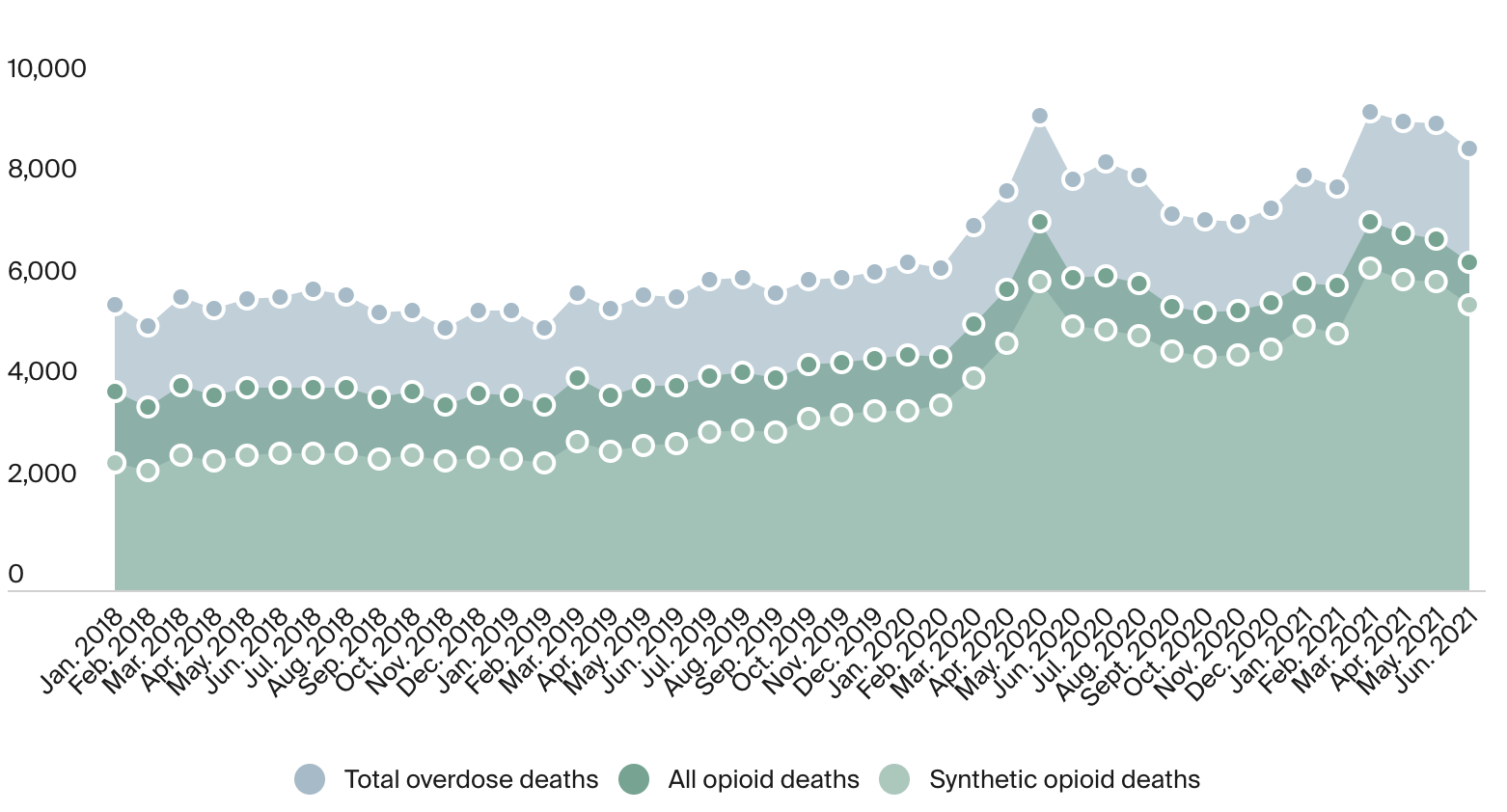
The lethal and volatile nature of the unregulated drug supply is a public health emergency. It must be treated as such, with quick and effective strategies to reduce overdose risks immediately. Increasing access to drug checking technologies, which give individuals information about the contents of their drugs prior to use, can reduce overdose deaths by alerting users to the presence of fentanyl and encouraging safer behavior.
Since 2018 at least 17 states have legalized possession and use of drug checking technologies. In April 2021, the U.S. Department of Health and Human Services authorized funding for drug checking, signaling the growing support for pragmatic and immediate interventions.[6] These are promising developments, but barriers to drug checking and other overdose prevention tools remain throughout the country.
A Need Created by Prohibition
The overdose crisis, tragic and terrifying as it is, is a predictable consequence of the United States’ drug strategy, which has long relied on prohibition and criminalization to suppress the sale and use of unregulated drugs. The evolution of the current epidemic reveals the failures of this approach.
At the start of the 21st century, prescription opioids became ubiquitous in family medicine cabinets and on street corners as pharmaceutical companies urged doctors to alleviate Americans’ untreated pain. But physical pain was not this country’s only collective affliction, and opioids soothe more than just a bad back or an injured knee. The increase in opioid prescribing dovetailed with pent-up demand for relief from more than physical suffering, including untreated mental illness and trauma, economic hardship, and the ennui of modern life. The public’s social and health care infrastructure, after decades of systematic neglect, could not meet the need for long-term solutions to these complex miseries. Instead, prescription painkillers offered a quick and effective salve.[7] They were also easy to get due to lax prescribing practices and rampant diversion of pills; individuals seeking opioids for recreation or self-medication could find them through friends, family members, or the illicit market.
By the mid-2000s, spikes in opioid-related overdoses in pockets of the country were causing alarm. The government response overwhelmingly focused on curtailing the availability of prescription opioids by forcing changes in prescribing and distribution practices, and the prescribed and diverted supplies of painkillers shrunk drastically. But there were no corresponding efforts to address demand by, for example, offering effective pain management alternatives or medically assisted treatment for opioid use.[8] Thousands of people dependent on opioids no longer had access to an unadulterated supply. Many of these individuals did not quit but instead turned to an unregulated supply chain that met demand first with heroin and then, around 2015, with fentanyl.
The Rise of Fentanyl
Fentanyl is a synthetic opioid used frequently and legitimately for surgical, acute, and severe pain, but it can also be manufactured illicitly with lab equipment. This means that unlike heroin, which is produced with opium derived from poppy plants, it is resistant to bad weather and crop eradication. Its potency means that small, easily transported, and hard-to-detect quantities yield high profits. These qualities make it well-suited to a market shaped by prohibition, which incentivizes drug adaptations (i.e., fentanyl instead of heroin) that benefit producers and suppliers, even when such adaptations heighten risks for consumers. It is impossible to know what the overdose crisis would look like today had our initial response not focused so singularly on reducing the availability of prescription opioids, but in the current environment, people who use drugs would be safer if they had access to a supply that is unadulterated and consistent in strength and quality.
Figure 2 — Counterfeit Pills Look Like the Real Thing
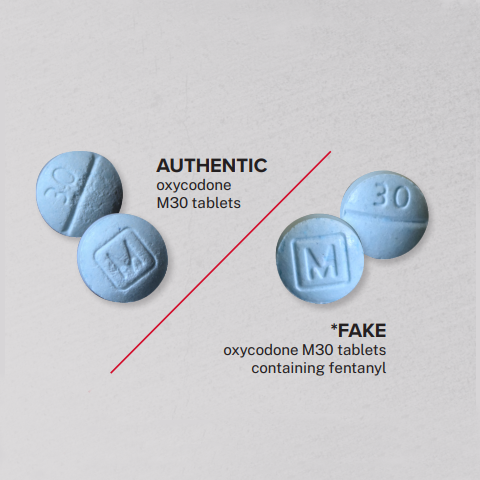
Fentanyl first started showing up in the drug supply in combination with heroin or in counterfeit prescription painkillers, which can be made with a pill press machine and materials purchased online. The risks of fentanyl exposure thus were limited initially to individuals who used opioids. But fentanyl is increasingly found in non-opioid illicit substances like cocaine and methamphetamine and in non-opioid counterfeit pills like benzodiazepines (e.g., Xanax or Valium) and stimulants (e.g., Adderall).[9] Opioids in combination with benzodiazepines (benzos) or with stimulants magnify the risk of overdose or other adverse events, especially for people with a low opioid tolerance. Individuals who purchase counterfeit benzos or stimulants may have little to no experience with opioids. They may assume the fake pills are authentic and likely do not expect them to contain fentanyl.
The growing prevalence of fentanyl in the non-opioid drug market expands overdose risks to a much larger population, including individuals who do not have substance use disorders and may use drugs only occasionally. Among teens, for instance, rates of drug use have been stable or declined over the past 20 years, but overdoses are now rising at a faster rate than for adults, due primarily to the proliferation of fentanyl in other unregulated drugs.[10] Such trends underscore the urgent need for drug checking.
Tools for Community-Based Drug Checking
Drug checking for user safety has been practiced in various settings since the 1960s. In the 1990s, several European countries, led by the Netherlands, started providing drug checking in response to rising use of new psychoactive substances at parties and festivals.[11] Over the past five years, it has received greater attention and support from law enforcement officials, public health agencies, and community service providers as a way to stem the tide of fentanyl-related deaths. Among the various technologies for drug checking, fentanyl test strips have quickly become the primary focus for policymakers.
Fentanyl test strips (FTS) are small strips of paper that have been treated to be highly sensitive to the presence of fentanyl and its analogues.[12] When dipped in water containing a small amount of drug residue, the strip will display one line if fentanyl is present, and two lines if it is absent. Results are provided within minutes.[13] The strips are inexpensive ($1-$2 per strip) and detect fentanyl with high accuracy.[14] Individuals report finding them easy to use and express a willingness and desire to use the strips to avoid fentanyl.[15] Test strips are also available to detect the presence of several types of benzodiazepines, a needed capability given their prevalence in the unregulated drug supply and frequent involvement in overdoses.[16] A growing number of service providers use and distribute benzo test strips, but they remain less utilized and less studied relative to fentanyl test strips.
Figure 3 — BTNX Fentanyl Test Strip Kit

Their accuracy and convenience make test strips a useful tool for addressing the overdose crisis. But they have limits, namely that they cannot identify the quantity of a substance in a sample and can only detect a single class of drug (i.e., fentanyls or benzos). While fentanyl is of the greatest concern today, it would be short-sighted to focus drug checking on one substance alone, as there is a rapidly evolving milieu of new psychoactive substances chemically engineered to mimic the properties of other well-known drugs.[17] For instance, a non-fentanyl-related opioid called isotonitazene and a sedative called xylazine have recently been identified in unregulated drugs, often in combination with other opioids. Both contribute to overdoses and other adverse events; neither can be detected with a fentanyl test strip.[18]
Based on past and current drug market trends, there is a high likelihood that a substance more lethal than fentanyl will emerge in the future. This necessitates access to and further development of more tools beyond test strips.
A handful of programs around the U.S. now offer drug checking with Fourier-transform infrared (FTIR) spectroscopy. Widely used for chemical analysis, FTIR spectroscopy identifies substances by measuring the way that infrared light is absorbed by a sample. It provides results in minutes and can identify numerous substances, including common unregulated drugs and cutting agents.[19] The equipment is mobile and can be used at events or in a service van. A single machine costs roughly $40,000, making it an expensive purchase for most community service providers, who also must be trained in how to operate it.[20] While FTIR analysis can detect multiple substances, it is less sensitive to fentanyl compared to the test strips, meaning the quantity of fentanyl in a sample has to be higher for FTIR equipment to identify it.[21] For this reason, many service providers with FTIR spectroscopy capabilities also use test strips to maximize information for clients.
Figure 4 — FTIR Spectrometer

Source Bruker.
Test strips and FTIR spectroscopy offer people a way to learn about the contents of their drugs quickly. Test strips detect fentanyl with high accuracy and can be distributed for at-home use; FTIR analysis can detect multiple substances and provide some information about the concentration of a compound in a sample.[22] Increasing access to and use of these tools is essential to the nation’s overdose response. At the same time, their limitations indicate a need to invest in developing advanced drug checking technologies that are inexpensive, easy to use, and provide fast results.
Drug Checking: Knowledge is Power
Real-time knowledge gleaned from drug checking empowers individuals to make more informed decisions about their drug use.
Several studies show that drug checking leads to positive behavioral changes that reduce overdose and other drug-related risks.[23] In surveys of drug users at music festivals and raves, between one- and two-thirds say they will not consume a substance if it is found to contain a “hazardous” compound.[24] While drug-dependent individuals may be less likely to abstain from use, they are more likely to reduce consumption, use more slowly, alter route of administration, or make other modifications that reduce risks.[25] A survey of people who inject drugs in North Carolina who were given FTS found that those who had a positive fentanyl test result were 5 times more likely to report changing their drug using behavior compared to those whose drugs did not test positive for fentanyl.[26] In San Francisco, over a quarter of injecting drug users whose drugs tested positive for fentanyl reported refraining from use, and 30% used less or did a test dose.[27] Several other analyses of drug checking programs similarly have found positive results for fentanyl to be associated with risk-reducing behavior modifications.[28]
Individuals who receive test strips from service providers often report giving them to others or sharing information about checked drugs with peers, suggesting that peer-to-peer distribution is an effective outreach strategy.[29] Providing test strips in bulk for at-home use, in addition to offering privacy and convenience, facilitates these positive network effects.
Pairing drug checking with interventions like naloxone and syringe distribution can enhance overdose mitigation by encouraging mutually reinforcing risk-reduction behaviors.[30] Drug checking also creates a pathway for engaging clients and connecting them with other services, including Hep C/HIV testing and care and substance use treatment.[31]
The utility of FTS may decrease for opioid users in fentanyl-saturated markets. These individuals would benefit from more robust drug checking options like FTIR analysis. But even in such environments, test strips are useful for confirming suspicions that drugs contain fentanyl, information that guides decisions like when and how much to use or whom to buy from.[32] Skeptics may argue that FTS enable people to “seek out” fentanyl, but this criticism ignores how individuals may come to prefer fentanyl in the first place—through repeated and unknowing exposure to the powerful drug, which increases their tolerance and renders less potent opioids too weak to prevent the onset of agonizing withdrawal symptoms. Withholding access to drug checking and the information it provides increases the likelihood of accidental and repeated fentanyl exposure.[33] On the other hand, drug checking can prevent fentanyl use, especially among newer users, by identifying its presence and empowering individuals to avoid it.
For people who sell drugs, drug checking can help reduce risks for clients. The average seller has incomplete or unreliable information about the substances being sold. Many use themselves and sell to friends or acquaintances and have both moral and economic reasons for not wanting customers to die.[34] An FTIR spectroscopy device can provide information on the strength of a batch of drugs containing fentanyl as well as information on other compounds that may increase risks for overdose or other adverse events.[35] Checking drugs prior to the point of retail sale could thus reduce drug-related harms for a larger population of users. Clearly, criminalization of drug sales impedes this activity, and it would be naïve to expect a U.S. jurisdiction to decriminalize the sale of drugs at this time. This reality makes it all the more important to identify and contend with the myriad ways in which prohibition increases user risks and obstructs efforts to lower those risks.
Drug Checking Does Not Encourage Drug Use
A common objection to drug checking is that it encourages drug use. This is the same charge leveled against syringe service programs and overdose prevention centers (also called safe injection sites), despite there being no evidence that any of these programs increase drug use. Countless factors may affect an individual’s decision to use or not use drugs, but the availability of a test strip or a needle is rarely, if ever, part of that calculation. By this same token, people who want to use drugs will use those drugs anyway—with or without drug checking or any other risk-reducing products. In the same way that passing out free condoms does not promote sex, drug checking does not promote drug use, but it does encourage safer behavior.
Fears that drug checking will enable drug use, while not based on evidence, are understandable. Drug checking and other harm reduction services operate from the position that some people want to use drugs and are not ready or do not want to stop. This is an unpalatable truth in a country that has long regarded abstinence as the only acceptable alternative to addiction. The idealization of abstinence is a byproduct of the war on drugs, which has taught generations of Americans that zero tolerance is the only way to stop people from getting high. But drug use, addiction, and death—not to mention racial inequality, incarceration rates, and violence along the southern border—have all increased alongside the drug war, demonstrating with painful clarity that prohibition and punishment do not work.
Drug Checking Best Practices
- Offer multiple drug checking tools, including fentanyl and benzo test strips and FTIR analysis, and provide training on how to use them.[36]
- Guarantee anonymity to service users.[37]
- Meaningfully include people with lived experience in implementation of and community outreach about drug checking services.[38]
- Develop and tweak as needed strategies for sharing test results with clients. Include qualitative information about how a substance looks, smells, feels, etc., to increase user knowledge.[39]
- Offer FTIR analysis and test strips in conjunction with other drug and behavioral health services in brick-and-mortar locations and mobile units.
- Offer on-site drug checking at music events to connect with individuals who may not frequent the same places as opioid-dependent populations.[40]
- Make test strips available on school campuses and in pharmacies, hospitals, libraries, bars, and night clubs to reach occasional users, friends and family of users, and the broader public.
- To further increase access, house test strips and other harm reduction products (naloxone, condoms, etc.) in secure vending machines that provide convenience and anonymity.[41]
- When feasible, partner with a lab for more advanced liquid or gas chromatography-mass spectrometry (LCMS/GCMS) testing to confirm that point-of-care testing is providing accurate results.[42]
- When feasible, pair drug checking implementation with an evaluative component that studies program effectiveness and strategies for optimizing service delivery.[43]
Legalizing Drug Checking: Policy and Political Calculations
Drug war–era policies prevent access to drug checking, which remains illegal in at least 25 states despite a recent wave of reform. In 1979, the Drug Enforcement Administration (DEA) produced the Model Drug Paraphernalia Act to address shortcomings in state efforts to prohibit paraphernalia. Over the next decade, at least 38 states adopted the comprehensive language of the DEA’s model act, which includes anything that can be used to “test” or “analyze” illicit substances.[44] As a practical matter, someone who purchases test strips online and uses them in the privacy of their own home is highly unlikely to face prosecution for violating a state’s paraphernalia laws. But state bans prevent formation of larger community distribution programs and block access to federal grant dollars for drug checking.
Fortunately, lawmakers are recognizing the need to update paraphernalia laws, and in the past four years at least 17 states have adopted provisions that allow drug checking. Some, like Arizona, Louisiana, Minnesota, and Tennessee, maintain all paraphernalia prohibitions and carve out exceptions only for fentanyl testing equipment. Others, including Maryland, Nevada, New Mexico, North Carolina, and Oklahoma, have implemented broader exemptions for drug testing technologies that permit more robust and flexible drug checking programs.[45]
The magnitude of the overdose crisis has blurred traditional partisan lines, and successful efforts to legalize drug checking in red states, albeit usually in a narrow fashion, indicate some consensus on this issue. But a polarized political climate threatens the delicate bipartisan support for drug reform. For example, conservative officials often blame the rise in fentanyl-related deaths on President Joe Biden’s border policies, even though these deaths were increasing well before he took office, climbing 490% between 2015 and 2020.[46] In Kansas, which had one of the greatest increases in overdose deaths among all states from 2021 to 2022, the Republican-led legislature rejected a bill to legalize fentanyl test strips.[47] Similar measures failed recently in Florida, Mississippi, and Missouri, all of which have rising rates of overdose deaths and are controlled by Republicans.
Stigma toward people who use drugs, false assumptions about drug use, and skepticism of harm-reducing interventions drive much of the resistance to reform. But political calculations are also a factor. Republican incumbents in solid-red districts may reason that drug reform is not a top priority for most of their primary voters, and that supporting drug checking or other harm reduction legislation could make them vulnerable to far-right challengers depicting them as weak on crime and the border. Conversely, measures like increasing penalties for possessing fentanyl and charging with homicide individuals who provide drugs to a person who fatally overdoses are popular among conservatives.[48] These actions will not reduce deaths, but they may give the appearance of responding to the crisis and punishing those responsible.
If the nation’s overdose response strategy continues in a patchwork fashion, it is reasonable to expect overdose trends to follow suit, declining in areas that take needed action and increasing in those that do not. Worsening geographic disparities in how people who use drugs are treated will exacerbate existing inequities that cut along racial, ethnic, and socioeconomic lines. Nationwide, overdose rates among Black and Hispanic/Latino populations are increasing faster than for white populations, but these trends are especially pronounced in the South and Southeast, regions that have been slow to respond to the crisis.[49] American Indian/Alaskan Native populations have the highest rates of overdose death and often live in rural areas lacking in health care, harm reduction, and drug treatment services.[50]
Figure 5 — U.S. Drug Overdose Rate per 100,000 People, by Race and Ethnicity
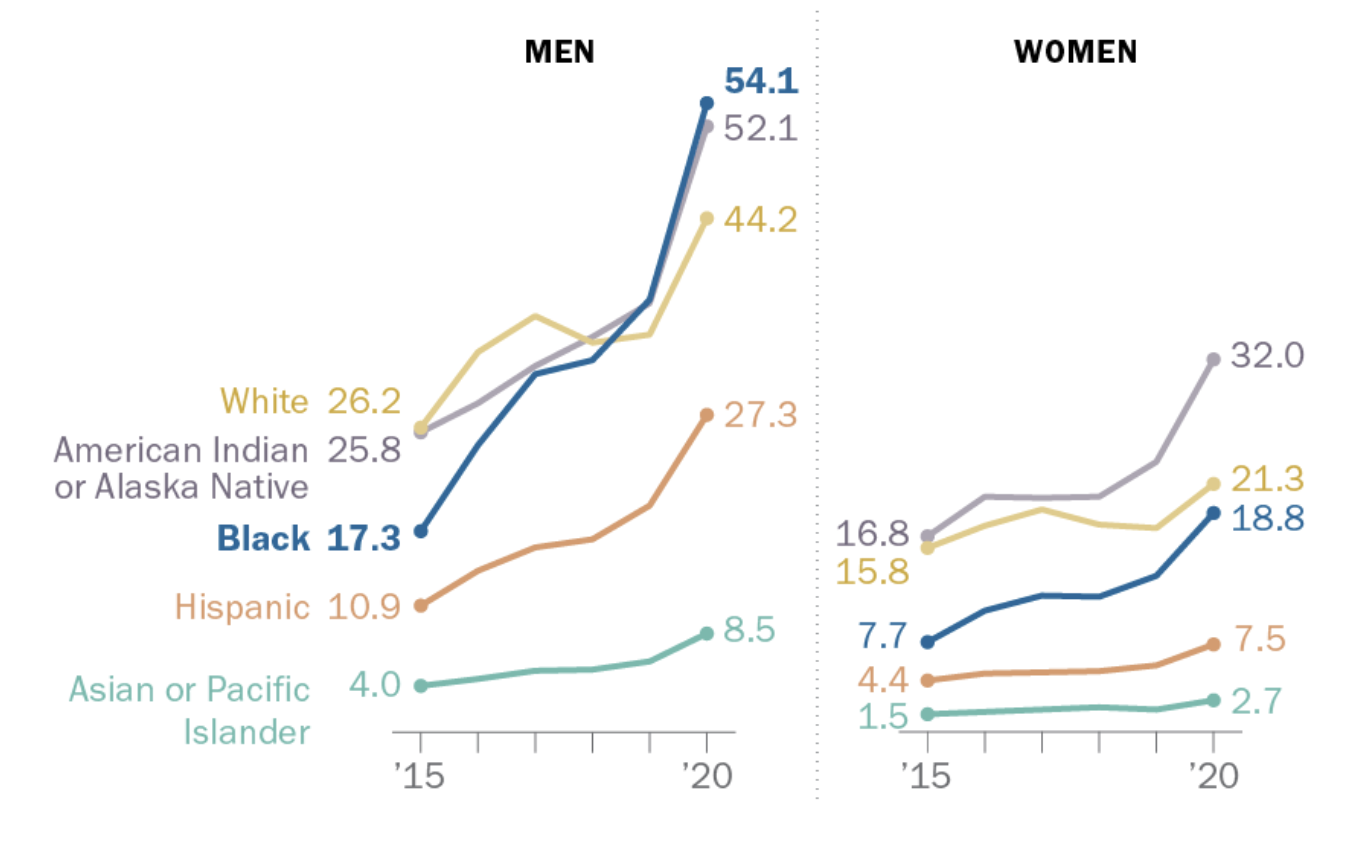
Inequities in service access expose the intersections between the overdose epidemic and inadequate health care, systemic racism, and socioeconomic inequality. Even when policymakers want to reach marginalized populations, they face entrenched challenges because of structural barriers built around race, place, class, and identity. Resistance from elected officials worsens these obstacles, and it is not a coincidence that many of the states lagging in drug reform also have some of the nation’s highest rates of poverty and incarceration and lowest rates of health insurance coverage.
Federal leadership could help move states in the right direction. The Biden administration has listed harm reduction as a top priority, and the Office of National Drug Control Policy, working with the Legislative Analysis and Public Policy Association, will soon release model legislation on drug checking, as it has for syringe service programs and overdose response.[51] States could be incentivized to adopt recommended reforms with a carrot-and-stick approach that offers funding to states that make changes and withholds it from those that do not. Congress routinely uses such incentives and has done so with drug policies; a 1991 law, for example, required states to enact laws suspending the driver’s license of anyone convicted of a drug offense in order to receive federal highway funds.[52] Such decisive action is unlikely at this time, however. Congressional dysfunction, deference to law enforcement, and political polarization make it difficult to predict when, or if, the nation’s drug strategy will shift toward preventing harm instead of causing it.
Conclusion
During recent debates in the Kansas state senate over a since-failed attempt to legalize fentanyl test strips, Republican state Senator Kellie Warren, who opposed the bill, said, “The best warning to figure out whether your drug might have fentanyl in it is, you know, don’t buy the illegal drugs… Where’s the personal accountability in this policy?”[53] Personal accountability, in the case of an accidental fentanyl exposure, can mean death. But people make mistakes, especially when they are young. And there are few parents who would view their own child’s death from an overdose as an acceptable price to pay for a questionable decision.
Whether the goal is to prevent overdoses, treat addiction, or stop kids from using drugs, all effective drug strategies require empathy and compassion for human suffering. Even before COVID-19, America had a deficit of these resources, and the pandemic has further stretched our capacity for caring, leaving little surplus for what may seem to many like consequences that result from discretionary and irresponsible individual behaviors. Until we can evolve into a society that is more inclusive of different ways of being and commits to easing human suffering, drug checking technologies offer a means to reduce deaths that result from adulterated drugs. This is good news for a problem that has been intractable for so long. If only we could summon the empathy and compassion needed to garner the will of legislators to embrace the life-saving power that drug checking puts in people’s hands.
Endnotes
[1] “Provisional drug overdose death counts,” Centers for Disease Control (CDC), 2022, https://bit.ly/3Q5BtHk.
[2] Jesse C. Baumgartner, Evan D. Gumas, and Munira Z. Gunja, “Comparing overdose mortality rates across high-income countries,” (blog), The Commonwealth Fund, May 19, 2022, https://bit.ly/3bnQfdG.
[3] “Trends in drug overdose deaths involving illicitly manufactured fentanyls,” CDC, 2021, https://bit.ly/3HNr1PZ.
[4] PolitiFact, “Facebook posts stated on December 19, 2021...” 2021, https://bit.ly/3Cv973q.
[5] J. Friedman et al., “Trends in drug overdose deaths among US adolescents,” JAMA 327, no. 14, 1398–1400.
[6] Legislative Analysis and Public Policy Association (LAPPA), Drug paraphernalia: Summary of state laws, 2022, https://bit.ly/3zSSJuc; Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services, “Federal grantees may now use funds to purchase fentanyl test strips,” April 7, 2021, https://bit.ly/3QhQqWX.
[7] For information on links between poverty, unemployment, lack of health infrastructure, and overdoses, see Elizabeth Kneebone and Scott W. Allard, A nation in overdose peril, The Brookings Institution, September 25, 2017, https://brook.gs/3SxU155.
[8] Medication-assisted treatment (MAT) is the most effective treatment for opioid use disorder. In recent years the U.S. has worked to expand access to MAT, but during the first decade of the epidemic it did not.
[9] J.N. Park et al., “Fentanyl and fentanyl analogs in the illicit stimulant supply,” Drug and Alcohol Dependence, 2020: 218. Also see H. Oh et al., “Fentanyl self-testing in a community-based sample of people who inject drugs,” International Journal of Drug Policy, 2020: 82.
[10] Monitoring the Future, Trends in 30-day prevalence of use of various drugs, 2021 https://bit.ly/3SwZCZs.
[11] In 1998 the U.S.-based nonprofit DanceSafe began checking drugs at music events. Community drug checking is operational in at least 20 countries, including Australia, Canada, Germany, Portugal, Spain, and the U.K. David E. Smith, “Street drug analysis and community based drug programs,” Journal of Psychedelic Drugs 6, no. 2, 1974: 153-159, https://bit.ly/3QcFqtN; Thomas Kerr and Kenneth Tupper, Drug checking as a harm reduction intervention, British Columbia Centre on Substance Use (BCCSU), 2017, https://bit.ly/3OWpRW5.
[12] FTS can be purchased online through organizations like DanceSafe (https://bit.ly/3P6kwLW) and BunkPolice (https://bit.ly/3zM01hQ).
[13] Kerr and Tupper, “Drug Checking,” note 11, Detecting Fentanyl. Saving Lives, Johns Hopkins Bloomberg School of Public Health, https://bit.ly/3oQRBke.
[14] Test strips can detect fentanyl at concentrations as low as 0.100 mcg/ml. This threshold makes it more sensitive to fentanyl than some lab equipment and highly applicable to user-level drug quantities. Traci C. Green et al., “An assessment of the limits of detection, sensitivity, and specificity of three devices for public health-based drug checking,” International Journal of Drug Policy, 2020, https://bit.ly/3BQ2RVV.
[15] Maxwell S. Krieger et al., “Use of rapid fentanyl test strips among young adults who use drugs,” International Journal of Drug Policy, 61, 2018: 52-58, https://bit.ly/3QfSLS5; Jacqueline E. Goldman et al., “Perspectives on rapid fentanyl test strips as a harm reduction practice among young adults who use drugs,” Harm Reduction Journal 16, no. 3, 2019, https://bit.ly/3zUbrle; “Baltimore & the overdose epidemic,” Johns Hopkins Bloomberg School of Public Health, 2018 https://bit.ly/3BCCaUk.
[16] Benzos were involved in 17% of all drug overdose deaths from January 2019 to June 2020. “International Overdose Awareness Day, CDC, https://bit.ly/3zH6yul. Aaron Shapiro et al., Detection of etizolam, flualprazolam, and flubromazolam by benzodiazepine-specific lateral flow immunoassay test strips, British Columbia Centre on Substance Use, July 2020, https://bit.ly/3zCy0Ju. For directions on using benzo test strips, see https://bit.ly/3zIhNT9.
[17] Matthew K. Laing et al., “An outbreak of novel psychoactive substance benzodiazepines in the unregulated drug supply,” International Journal of Drug Policy, July 2021, https://bit.ly/3Sx0GfU.
[18] Marthe M. Vandeputte et al., “The rise and fall of isotonitazene and brorphine,” Journal of Analytical Toxicology 46, no. 2, March 2022: 115–121, https://bit.ly/3SpS1Mi; Andrew Joseph, “With overdoses at record highs, a veterinary tranquilizer spreading through the U.S. drug supply poses new threats,” STAT News, March 11, 2022, https://bit.ly/3SitZma; Jess Arnold, “DEA offers grim warning about new dangerous drug in D.C. region,” WUSA90, May 17, 2022, https://bit.ly/3bp928B.
[19] Brandon Yau et al., A field assessment of FTIR and FTS as point-of-care drug checking technologies, British Columbia Centre on Substance Use, https://bit.ly/3oQTgX0.
[20] Author’s communication with Bruker representative, July 7, 2022.
[21] Fentanyl must be present at levels of 10% concentration by weight to ensure reliable detection with FTIR spectroscopy. This is a somewhat high threshold for user-level drug quantities; see Yau et al., "A field assessment of FTIR," note 18, and Karen McCrae et al., “Assessing the limit of detection of FTIR and immunoassay strips for fentanyl in a real-world setting,” Drug Alcohol Review 39, no. 1, January 2020, https://bit.ly/3zPVpZu.
[22] Though FTIR spectroscopy testing can provide information on the concentration of a drug contained in the sample, this requires more training and is limited in scope, and some providers may not have enough confidence to share results with clients. Yau et al., A field assessment of FTIR, note 18.
[23] Ju Nyeong Park et al., “A fentanyl test strip intervention to reduce overdose risk among female sex workers who use drugs in Baltimore,” Addictive Behaviors, November 2020, https://bit.ly/3tHUoyb; Nicholas C. Peiper et al., “Fentanyl test strips as an opioid overdose prevention strategy,” International Journal of Drug Policy 63, 2019: 122–128, https://bit.ly/37ixar2; Krieger et al., “Use of rapid fentanyl test strips,” note 14.
[24] Kerr and Tupper, “Drug Checking,” note 11.
[25] Nazlee Maghsoudi et al, “Drug checking services for people who use drugs: A systematic review,” Addiction, 2021, https://bit.ly/3SHmlCe.
[26] Peiper et al., “Fentanyl test strips,” note 20.
[27] Oh et al., “Fentanyl self-testing,” note 9.
[28] Ju Nyeong Park et al., “Evaluation of fentanyl test strip distribution in two Mid-Atlantic syringe service programs,” International Journal of Drug Policy, 2021, https://bit.ly/3QgJtVV; Krieger et al., “Use of rapid fentanyl test strips,” note 14; Kerr and Tupper, “Drug Checking,” note 11; Park et al., “A fentanyl test strip intervention,” note 20.
[29] N.P. Weicker et al., “Agency in the fentanyl era: Exploring the utility of fentanyl test strips in an opaque drug market,” International Journal of Drug Policy 84, 2020; Goldman et al., “Perspectives on rapid fentanyl test strips,” note 14; Maghsoudi et al., “Drug checking services,” note 22.
[30] See Oh et al., “Fentanyl self-testing,” note 9.
[31] J.J. Carroll et al., “The Bronze Age of drug checking: Barriers and facilitators to implementing advanced drug checking amidst police violence and COVID-19,” Harm Reduction Journal 19, no. 9, 2022.
[32] Park et al., “Fentanyl self-testing,” note 20; Goldman et al., “Perspectives on rapid fentanyl test strips,” note 14; Weicker et al., “Agency in the fentanyl era,” note 29.
[33] Weicker et al., “Agency in the fentanyl era,” note 29.
[34] Geoff Bardwell et al., “The potential role of drug dealers in reducing drug-related harms via drug checking,” Drug Alcohol Dependence 198, 2019: 1–6, https://bit.ly/3Sreys3.
[35] Alex Betsos et al., “A rapid ethnographic study of drug sellers’ use of drug checking,” International Journal of Drug Policy, 2021, https://bit.ly/3JtWhWH; Carroll et al., “The Bronze Age of drug checking,” note 31.
[36] For an example of instructions on how to use test strips, see “How to Test Your Drugs,” New York City Health Department, https://on.nyc.gov/3Q5yrDj.
[37] Maghsoudi et al., “Drug checking services,” note 22.
[38] Bruce Wallace et al., “What is needed for implementing drug checking services in the context of the overdose crisis?,” Harm Reduction Journal 17, no. 29, 2020: https://bit.ly/3zUCb4K.
[39] This helps avoid what Nabarun Dasgupta and Marcy Figgatt call “tyranny of the molecule,” in which primacy is given to molecular information over human understanding; see https://bit.ly/3Q05rN9.
[40] Ines Hungerbuehler et al., “Drug checking: A prevention measure for a heterogenous group with high consumption frequency and polydrug use,” Harm Reduction Journal 8, no. 16, 2011, https://bit.ly/3oOo8Yp.
[41] Harm-reduction vending machines are being deployed in Ohio (https://bit.ly/3BWC8a7), New York (https://bit.ly/3AinKbf), and Canada (https://bit.ly/3bNjlmV).
[42] LCMS and GCMS testing provide detailed quantitative information on drug samples, but equipment is costly, analysis requires highly trained technicians, and results are not immediate. See Kerr and Tupper, “Drug Checking,” note 11.
[43] Unanswered questions relate to drug checking, among other things including demographic profiles of populations who utilize services; whether historically disadvantaged groups have equal access; the short- and long-term effects of DCS on behavior; and optimal methods for communicating information to users and the public.
[44] LAPPA, Drug Paraphernalia, note 6.
[45] Id.
[46] National Institute on Drug Abuse, Overdose death rates, 2022, https://bit.ly/3Jtb3Ny; Jeremy Wallace, “While border patrol seizes record amounts of fentanyl, Gov. Abbott attacks Biden for ‘doing nothing,’” Houston Chronicle, March 12, 2022, https://bit.ly/3btVada; Andrew Olivastro, “Fentanyl’s wake,” Heritage Foundation, May 27, 2022, https://herit.ag/3Jq9Gzf.
[47] CDC, note 1.
[48] For example, see Sara Carter, “Outrageous House Democrats block fentanyl trafficking bill,” February 3 2022, https://bit.ly/3BHgiaI; Shannon Najmabadi and Jesse Paul, “Here’s what’s in the Colorado fentanyl ‘accountability and prevention’ bill just signed into law,” Colorado Sun, May 11, 2022, https://bit.ly/3d4BOLX; Maria Clark, “As fentanyl deaths spike in Mississippi, new law imposes harsher penalties on dealers,” Mississippi Clarion Ledger, April 20, 2022, https://bit.ly/3QfCe0v.
[49] T. Townsend et al., “Racial/ethnic and geographic trends in combined stimulant/opioid overdoses, American Journal of Epidemiology 191, no. 4, March 2022: 599–612.
[50] Holly Hedegaard et al., Drug overdose deaths in the United States, NCHS Data Brief No. 428, 2021, https://bit.ly/3QjvhM4.
[51] White House Briefing, White House releases model law to help states ensure access to syringe service programs, 2021, https://bit.ly/3Sp2OGw; LAPPA, Drug Paraphernalia, note 6.
[52] The Solomon-Lautenberg Amendment, https://bit.ly/3PWRa3L. The amendment allowed for states to opt out of compliance through a formalized process. The Drug-Free Workplace Act of 1988 also requires all federal contractors and grantees, including state agencies, to guarantee a drug-free workplace as a precondition for receiving funds (https://bit.ly/3OVGzF1).
[53] Noah Taborda, “As opioid overdoses spike in Kansas, senators block fentanyl test strip provision,” Kansas Reflector, May 2, 2022, https://bit.ly/3dLGve4.
This material may be quoted or reproduced without prior permission, provided appropriate credit is given to the author and Rice University’s Baker Institute for Public Policy. The views expressed herein are those of the individual author(s), and do not necessarily represent the views of Rice University’s Baker Institute for Public Policy.



