Making Stem Cell Interventions and Advertisements Safer and More Effective in Texas

Table of Contents
Author(s)
Akshaya Venkatesh
Graduate Student Intern, Center for Health and Biosciences
Kirstin R.W. Matthews
Fellow in Science and Technology PolicyShare this Publication
- Print This Publication
- Cite This Publication Copy Citation
Akshaya Venkatesh and Kirstin R.W. Matthews, "Improving Stem Cell Safety in Texas: Making Stem Cell Interventions and Advertisements Safer and More Effective in Texas-based Stem Cell Clinics" (Houston: Rice University’s Baker Institute for Public Policy, September 6, 2022), https://doi.org/10.25613/H0ZQ-9Q28.
Tags
Introduction
Stem cells have two unique properties that make them an appealing therapeutic tool for regenerative medicine: they can grow indefinitely and can differentiate into a wide variety of cell types, including those that form blood, bones, lungs, skin, and the brain.[1] Different examples of stem cells include embryonic stem cells (obtained from an embryo); induced pluripotent stem cells (created in a lab from normal cells, such as skin cells); and stem cells that are naturally found in the human body, such as those in bone marrow. Because of their regenerative potential, stem cells are a frequent and promising area of research for a wide range of conditions.[2]
Stem cell interventions (SCIs) have been used in clinics around the world for the past 20 years. More than 2,700 SCI clinics have been identified in the United States, with Texas having one of top three number of locations in the country.[3] These clinics market SCIs to treat or cure multiple diseases and disorders, such as orthopedic, neurologic, and autoimmune conditions.[4] While some SCIs have been approved for blood diseases and cancers, most SCIs are still being studied, and some are in clinical trials and have not been approved by a regulatory authority. Thus, these interventions are considered experimental.[5]
Figure 1 — The Increasing Number of Stem Cell Clinics in the United States and Texas
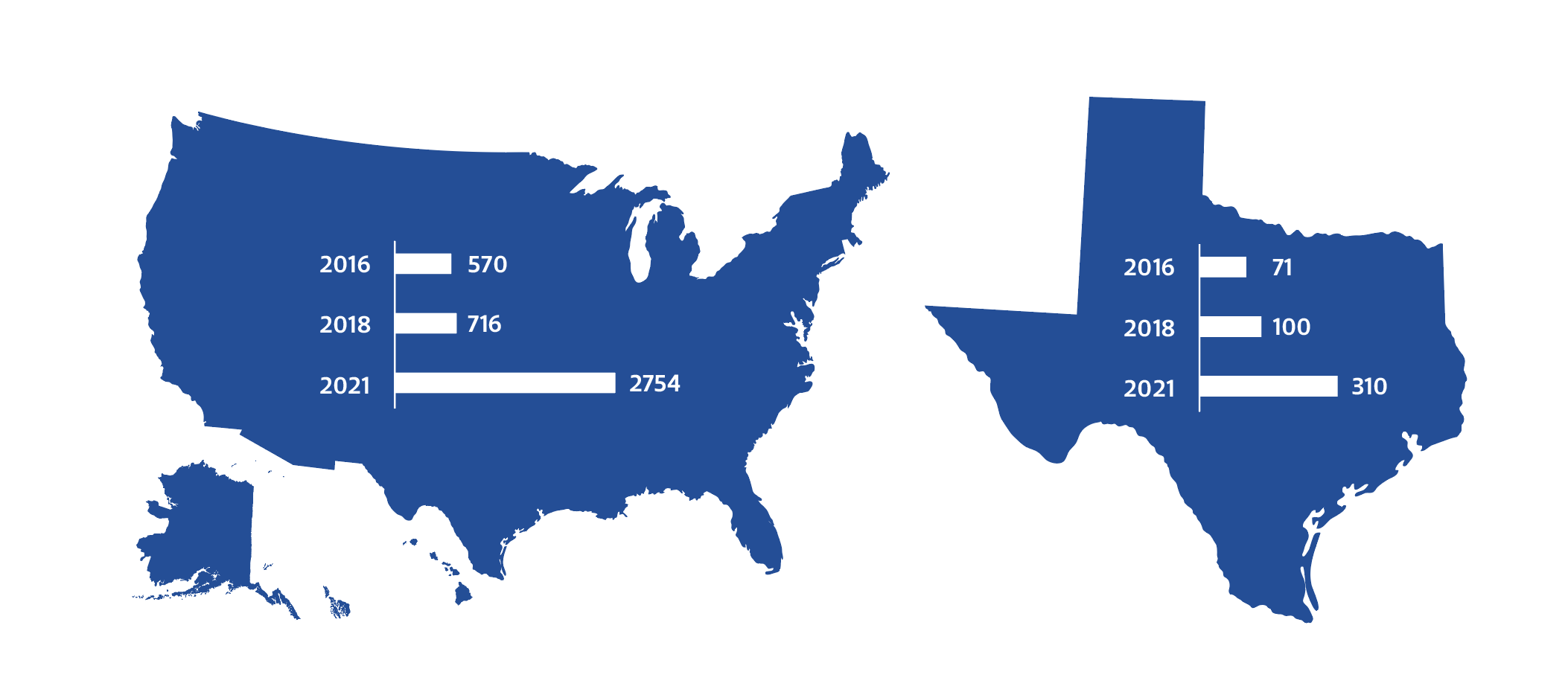
In 2017, state lawmakers enacted Texas House Bill 810 to increase patient access to experimental SCIs for chronic or terminal illnesses.[6] However, patients do not always receive notice prior to treatment that some SCIs are experimental and might carry a higher risk than those approved by the U.S. Food and Drug Administration (FDA). In this brief, we discuss the risks of experimental SCIs and offer recommendations for ways to increase patient awareness of the risks before treatment to improve market safety.
The Risks and Benefits of SCIs
SCIs offer hope to individuals with debilitating diseases and limited opportunities for relief. However, results so far are mixed. Some patients have received positive results from SCIs, promoting further use in certain cases. Other patients have reported severe side effects from the procedure including sepsis, blindness, tumors, and even death.[7] Stories of uninformed patients experiencing negative side effects from SCIs conducted by unscrupulous providers have emerged across the country, including in Texas, as detailed in 2020 by Texas Monthly.[8]
The article reported that in 2018, Dorothy O’Connell underwent an SCI for arthritis at a small clinic in Missouri City, Texas.[9] Neither O’Connell nor her daughter who accompanied her to the appointment were aware that the injections were not approved by the FDA. Unfortunately, the stem cells used in the treatment were contaminated. O’Connell, and multiple other patients across Texas and the United States who used the same stem cell product, developed debilitating bacterial infections.
This incident highlights the risk associated with SCIs. It also illustrates how patients receiving SCIs might not fully understand that the procedures are experimental or all the risks associated with these procedures. SCI advertisements often provide the reader with misleading and at times false information related to the risks and benefits of the procedure, making it difficult for the public to discriminate between accepted medical practice and unproven interventions.[10] Efforts by consumers to find safe and effective treatments are further complicated by less scrupulous clinics that promote their SCIs by only referencing certain aspects of biomedical and clinical research, as well as clinical regulation.
Commonly referred to as “tokens of legitimacy,” these tactics create the appearance of legitimacy, and may mislead patients to receive an SCI (Table 1). Unfortunately, the FDA does not moderate clinicaltrials.gov; therefore, any company can register their pay-to-participate trials on this website without any regulatory board overseeing the posting of these trials.[11] Clearly, the practice of registering trials without professional oversight hinders the ability of patients to separate legitimate trials from those without FDA approval, and falsely suggests to patients that an experimental SCI is government-approved. Other misleading tactics include patient videos emphasizing a positive outcome following an SCI, and omitting any reference to severe or prevalent negative results. Clinics also include links to scientific papers that may be published without peer review, which can put the papers’ validity into question or papers that do not scientifically support a clinic’s treatment, such as animal studies; such studies might be easy for patients to overlook.
Table 1 — Creating an Appearance of Scientific Legitimacy
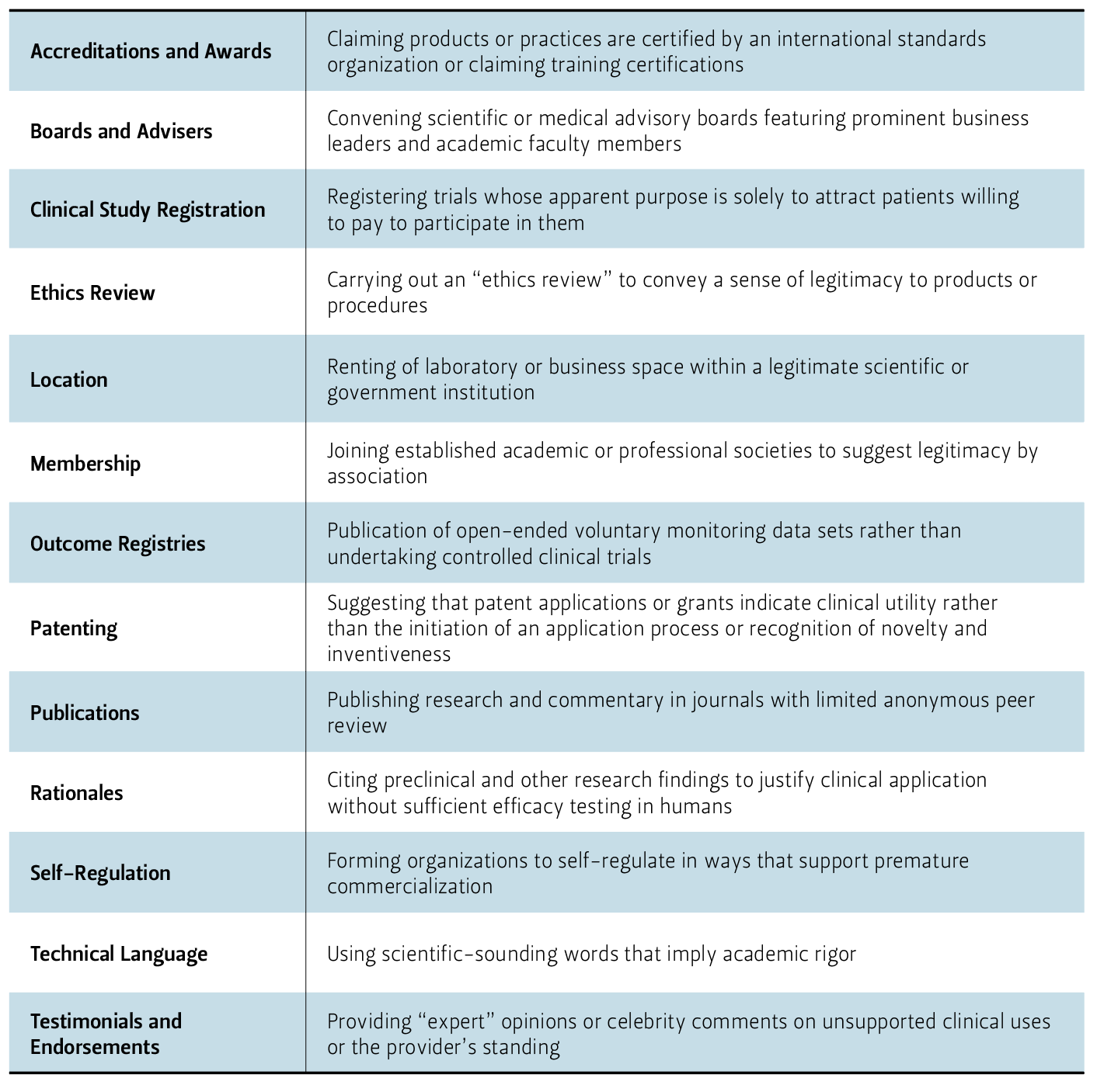
Businesses offering SCIs sometimes reference the FDA in their advertisements, but not necessarily in a manner that describes the FDA’s stance on experimental SCIs or that includes any related safety issues.[12] Presenting a connection to the FDA, but not stating the experimental nature of these treatments, can cause patients to believe that these treatments are approved by the FDA or have support from the FDA, increasing their legitimacy. Such “tokens of legitimacy” cause patients to receive misleading information, as in O’Connell’s case.[13] Fortunately, some online companies, such as Google, have implemented advertising policies that limit or eliminate the marketing of non-FDA approved SCIs.[14] Advertising that accurately portrays the current status of SCIs will help patients make informed decisions.
While clinics may register their treatments as clinical trials, they often do not accurately report the results, leading to more misinformation for patients. Furthermore, studies have demonstrated that patients who research stem cell clinical trials are more frequently exposed to positive results, rather than to studies that show no difference in the condition or a negative result.[15] What’s more, research showing positive results is more likely to be published than studies showing the SCI had no impact or negative side effects. In reality, researchers estimate that nearly half of patients who undergo an SCI will likely gain no benefit or will experience negative side effects, along with their original condition.[16] By not presenting negative or inconclusive results from these studies, the public does not have a full picture of the results and may not have a complete understanding of the negative consequences that can arise.[17]
Patients require additional protections when seeking the experimental therapies that are currently allowed under Texas law. While some patients who undergo SCIs may develop harmful conditions, such as severe infections, tumors, and blindness, clinics are not required to provide specific information about their therapies; and accessible resources for patients or regulators to evaluate specific providers do not exist.[18] Companies that provide SCIs do not report negative consequences for SCIs on advertisements or websites, which further hinders patient access to information about safety. Improving advertising, such that information accurately portrays the current regulatory status of SCIs and creating a public database of treatment outcomes will ensure that patients have the information necessary to make an informed decision.
Recommendations
While many clinics and physicians offer experimental SCIs hopes of providing a new solution for a severe chronic illness or injury, less scrupulous actors are using the technology without regard to patient safety. To prevent unnecessary risks and to better inform patients about SCIs, we propose three recommendations for improved patient safety and awareness in Texas.
Recommendation 1: Display disclaimers at clinics that SCIs are experimental.
Clinics that provide experimental SCIs should present a clear statement that acknowledges that their SCIs have not obtained FDA approval and are experimental. This statement should be displayed by the entrance of the clinic and in the physical space where the SCI treatment is provided. This display will ensure that patients more fully understand the current state of research behind stem cell treatments and can make informed decisions before proceeding with the intervention. A recommended statement is: “This clinic offers stem cell-based interventions. These therapies have not been approved by the U.S. Food and Drug Administration and are considered experimental.”
Displaying disclaimers in clinics can also invite conversations between patients and their primary physicians regarding the safety and efficacy of SCIs prior to treatment. If patients see signs stating the experimental nature of this therapy, they may be more inclined to talk to their primary care physician about whether the treatment will be beneficial for them. Creating a prompt for patients to engage with physicians with questions and concerns regarding SCIs further allows for increased patient education prior to the administration of SCIs.[19] Physicians should take care to avoid misleading a patient further and should assist in separating the appearance of legitimacy from scientific information. Experts in the field propose that physicians follow three criteria when discussing unproven therapies such as SCIs with patients—especially patients who may feel they are out of options: (1) ensure, if true, that the SCIs at the clinic have not been shown to have harmful effects; (2) determine if the SCI might provide some form of benefit to the patient; and (3) reiterate that this therapy is still experimental, and may not relieve symptoms of their condition.[20]
Studies have found that many physicians do not keep up with the scientific literature related to SCIs and are therefore reluctant to provide comprehensive information to patients on this topic.[21] To better help physicians and patients who may be interested in learning more about SCIs, consulting services (such as the Mayo Clinic Regenerative Medicine Consult Services) offer reliable educational information and may be able to help connect them to resources suited for their condition. By using these resources and following the guidelines above, physicians are better prepared to talk to patients about SCI therapies, and patients can receive additional opinions prior to undergoing treatment.
Recommendation 2: Place a disclaimer on SCI advertisements that they are experimental.
Patients initially receive information about SCIs through online and print advertisements. For example, O’Connell and her daughter heard about SCIs through a local newspaper advertisement.[22] However, many SCI advertisements include a reference to the FDA, which implies the treatment has FDA approval.[23] Since these treatments are experimental and not regulated by the FDA, this advertising tactic is misleading.
Clinics who advertise SCIs for any condition should include a clear statement noting that the procedure and/or product is experimental. In 2007, Texas legislators passed House Bill 1676, which increased the safety of electronic prescription drug advertising by educating consumers about misleading statements by pharmacies or pharmaceutical drug merchants. A similar disclaimer on SCI advertisements would let the patient know about potential risks and allow them to make a more informed decision. Recommended phrasing: “This stem cell-based intervention has not been approved by the United States Food and Drug Administration (FDA) and is considered an experimental therapy.” This clear statement, in a font the same size as the text of the advertisement, would promote patient awareness of the risks associated with the procedure and help them determine whether the risks are worth the potential benefits.
Recommendation 3: Report SCI adverse events to the Texas medical boards.
More than 400 patients experienced negative side effects after experimental SCIs, according to reports in the academic literature and popular press between 2004 and 2020.[24] These side effects ranged from infections, decrease in mobility, inoperable tumors and even death. However, many scholars believe more unreported events are likely to have occurred—but side effects may not have been properly linked to the SCI.
Reporting adverse events in a registry would allow patients to identify clinics and stem cell-based products with questionable safety records. In 2018, Liveyon—the company that sold the stem cell-based product O’Connell received—had to remove the product from the market due to adverse effects in patients.[25] If physicians and clinicians are required to report instances where patients experience side effects from stem cell-based products, then SCIs can be used in the safest possible manner.
The FDA Adverse Events Reporting System (FAERS) currently has a way to report negative side effects. However, FAERS does not capture all adverse events because clinicians are not required to submit reports if they are only treating a patient’s side effects and they do not know all the information regarding the particular SCI that a patient received. This makes the FAERS system less effective.[26] By requiring not only the doctors who treat patients with SCI side effects but also the clinics to report adverse events, the registry should capture a larger portion of negatively affected patients. Researchers have seen more side effects reported by patients on social media and other online platforms than by FAERS. Furthermore, reporting these events to state medical boards and having this information publicly available could supplement reports sent to FAERS on the state level, and minimize risks from unsafe clinics and SCIs. Providing more clarification on adverse events originating from SCI treatments allows consumers to be aware of a clinic’s outcomes.
Texas’ 2017 legislation included the requirement that SCI clinics report its procedures to the Texas State Medical Board.[27] In the following legislative session, this reporting start date was moved to 2027 from 2019. While this data might interest scholars, it will have a limited public health benefit. However, by changing the registry to also include reports starting in 2023 of adverse events each year, patients can identify potentially unsafe stem cell-based products or clinics.
Conclusion
SCIs offer hope to many patients facing serious chronic diseases and injuries. However, it is important that patients make informed choices when considering treatments for their health. Our recommendations are not intended to detract from patient autonomy or minimize a patient’s right to make their own health care choices. Rather, these recommendations are meant to allow patients to have as much information as possible about a given health care option. Disclaimer laws have been passed and implemented in other states, where notices are prominently displayed in clinics and on advertisement for SCIs, and Texas has previously sought to protect patients through similar laws for online pharmacies and prescriptions.[28] Furthermore, the reporting of adverse events would help identify procedures, products, or clinics that are markedly unsafe to ensure patients who choose to obtain experimental SCIs are as protected as possible.
These recommendations are in line with Texas HB 810 (2017), as they still allow experimental SCIs for patients suffering from chronic conditions—but they allow more education prior to patients making that choice.[29] To improve patient safety and education before the administration of SCIs, there should be increased awareness that SCIs are experimental and do not have FDA approval, and adequate reporting of adverse events associated with experimental procedures.
Acknowledgments
The authors would like to thank Leigh Turner for providing Texas- and U.S.-specific data on SCI clinics. We would also like to thank Nathan Cook, Ross Geisinger, Tyler Lamb, and Dan Wagner for reviewing and editing drafts of the manuscript. Funding for this project was generously provided by a grant from the Hamman Foundation and by the Center for Health and Biosciences and the Qatar Stem Cell Endowment.
Endnotes
[1] Zakrzewski, Wojciech, Maciej Dobrzyński, Maria Szymonowicz, and Zbigniew Rybak. 2019. “Stem Cells: Past, Present, and Future.” Stem Cell Research & Therapy 10 (1): 68. https://doi.org/10.1186/s13287-019-1165-5.
[2] Zakrzewski et al, “Stem Cells”; Tsai, Robert Y. L. 2016. “Balancing Self-Renewal against Genome Preservation in Stem Cells: How Do They Manage to Have the Cake and Eat It Too?” Cellular and Molecular Life Sciences 73 (9): 1803–23. https://doi.org/10.1007/s00018-016-2152-y.
[3] Turner, Leigh. 2021. “The American Stem Cell Sell in 2021: U.S. Businesses Selling Unlicensed and Unproven Stem Cell Interventions.” Cell Stem Cell 28 (11): 1891–95. https://doi.org/10.1016/j.stem.2021.10.008.
[4] Turner, “The American Stem Cell in 2021”; Guleria, Indira, Maria Los Angeles Muñiz, Matthew Wilgo, Asawari Bapat, Wanxing Cui, Yen‐Michael Sheng Hsu, Madhan Jeyaraman, et al. 2022. “How Do I: Evaluate the Safety and Legitimacy of Unproven Cellular Therapies?” Transfusion 62 (3): 518–32. https://doi.org/10.1111/trf.16814.
[5] Ibid.
[6]. Matthews, Kirstin, Bhavana Kunisetty, and Keri Sprung. 2018. “Texas H.B. 810: Increased Access to Stem Cell Interventions or an Increase in Unproven Treatments?” Stem Cells and Development 27 (21): 1463–65. https://doi.org/10.1089/scd.2018.0148.
[7] Knoepfler, Paul S, and Leigh G Turner. 2018. “The FDA and the US Direct-to-Consumer Marketplace for Stem Cell Interventions: A Temporal Analysis.” Regenerative Medicine 13 (1): 19–27. https://doi.org/10.2217/rme-2017-0115; Matthews, Kirstin R.W., Omar Kawam, Keri Sprung, Emerson C. Perin, and Zubin Master. 2022. “Role of Physicians in Guiding Patients Away From Unproven Stem Cell Interventions.” Texas Heart Institute Journal 49 (2): e217768. https://doi.org/10.14503/THIJ-21-7768; Turner, Leigh. 2018. “The US Direct-to-Consumer Marketplace for Autologous Stem Cell Interventions.” Perspectives in Biology and Medicine 61 (1): 7–24. https://doi.org/10.1353/pbm.2018.002.
[8] Beil, Laura. 2020. “How Unproven Stem Cell Therapies Are Costing Desperate Patients,” January 19.
[9] Ibid.
[10] Sipp, Douglas, Timothy Caulfield, Jane Kaye, Jan Barfoot, Clare Blackburn, Sarah Chan, Michele De Luca, et al. 2017. “Marketing of Unproven Stem Cell–Based Interventions: A Call to Action.” Science Translational Medicine 9 (397): eaag0426. https://doi.org/10.1126/scitranslmed.aag0426; Turner, “The American Stem Cell in 2021.”
[11] Sipp et al., “Marketing of Unproven Stem Cell-Based Interventions”; Snyder, Jeremy, and Leigh Turner. 2018. “Selling Stem Cell ‘Treatments’ as Research: Prospective Customer Perspectives from Crowdfunding Campaigns.” Regenerative Medicine 13 (4): 375–84. https://doi.org/10.2217/rme-2018-0007; Wagner, Darcy E, Leigh Turner, Angela Panoskaltsis-Mortari, Daniel J Weiss, and Laertis Ikonomou. 2018. “Co-Opting of ClinicalTrials.Gov by Patient-Funded Studies.” The Lancet Respiratory Medicine 6 (8): 579–81. https://doi.org/10.1016/S2213-2600(18)30242-X; Zarzeczny, Amy, Claire Tanner, Jan Barfoot, Clare Blackburn, Anna Couturier, and Megan Munsie. 2019. “Contact Us for More Information: An Analysis of Public Enquiries about Stem Cells.” Regenerative Medicine 14 (12): 1137–50. https://doi.org/10.2217/rme-2019-0092.
[12] Cook, Margaret, Alexandra Richey, David A. Brafman, and Emma K. Frow. 2021. “Weighing up the Evidence Used by Direct-to-Consumer Stem Cell Businesses.” Stem Cell Reports 16 (12): 2852–60. https://doi.org/10.1016/j.stemcr.2021.10.007.
[13] Beil, “How Unproven Stem Cell Therapies.”
[14] “Healthcare and Medicines - Advertising Policies Help.” Accessed July 28, 2022. https://support.google.com/adspolicy/answer/176031
[15] Fung, Moses, Yan Yuan, Harold Atkins, Qian Shi, and Tania Bubela. 2017. “Responsible Translation of Stem Cell Research: An Assessment of Clinical Trial Registration and Publications.” Stem Cell Reports 8 (5): 1190–1201. https://doi.org/10.1016/j.stemcr.2017.03.013.
[16] Daley, George Q. 2012. “The Promise and Perils of Stem Cell Therapeutics.” Cell Stem Cell 10 (6): 740–49. https://doi.org/10.1016/j.stem.2012.05.010.
[17] Fung et al. “Responsible Translation of Stem Cell Research.”
[18] Guileria et al, “How Do I”; Knoepler and Turner, “The FDA and US Direct-to-Consumer” ; Wagner et al, “Co-Opting of ClinicalTrials.Gov.”
[19] Matthews et al., “Role of Physicians.”
[20] Kawam, Omar, Jon C. Tilburt, and Zubin Master. 2021. “Physician Responsibility to Discuss Palliative Unproven Therapies With Out-of-Option Patients.” The American Journal of Bioethics 21 (12): 31–33. https://doi.org/10.1080/15265161.2021.1991038.
[21] Smith, Cambray, Aidan Crowley, Megan Munsie, Erin S. DeMartino, Nathan P. Staff, Shane Shapiro, and Zubin Master. 2021. “Academic Physician Specialists’ Views toward the Unproven Stem Cell Intervention Industry: Areas of Common Ground and Divergence.” Cytotherapy 23 (4): 348–56. https://doi.org/10.1016/j.jcyt.2020.12.011.
[22] Beil, “How Unproven Stem Cell Therapies.”
[23] Cook, et al., “Weighing up the Evidence.”
[24] Matthews et al., “Role of Physicians”; The PEW Charitable Trust. “Harms Linked to Unapproved Stem Cell Interventions Highlight Need for Greater FDA Enforcement,” June 1, 2021. https://www.pewtrusts.org/en/research-and-analysis/issue-briefs/2021/06/harms-linked-to-unapproved-stem-cell-interventions-highlight-need-for-greater-fda-enforcement.
[25] Beil, “How Unproven Stem Cell Therapies.”
[26] PEW “Harms Linked to Unapproved Stem Cell Interventions.”
[27] Matthews, Kunisetty, and Sprung, “Texas H.B. 810.”
[28] Akkas, Farzana, Leigh Turner, and Elizabeth Richardson. 2022. “Adverse Events Related to Unapproved Stem Cell Products and Other Regenerative Interventions: Recommendations for More Robust Regulation of the Direct-to-Consumer Marketplace.” Regenerative Medicine 17 (2): 63-68. https://doi.org/10.2217/rme-2021-0124.
[29] Matthews, Kunisetty, and Sprung, “Texas H.B. 81.0”
This material may be quoted or reproduced without prior permission, provided appropriate credit is given to the author and Rice University’s Baker Institute for Public Policy. The views expressed herein are those of the individual author(s), and do not necessarily represent the views of Rice University’s Baker Institute for Public Policy.]


