HRMS Issue Brief #3: Early Effects of the Affordable Care Act on Health Insurance Coverage in Texas for 2014

Table of Contents
Author(s)
Vivian Ho
James A. Baker III Institute Chair in Health EconomicsElena M. Marks
Senior Fellow in Health PolicyPatricia Gail Bray
The Episcopal Health Foundation | Adjunct Faculty, The University of Texas School of Public Health’s Fleming Center for Healthcare ManagementShare this Publication
- Print This Publication
- Cite This Publication Copy Citation
Ho, V., Marks, E., and Bray, P.G. James A. Baker III Institute for Public Policy, Rice University, The Episcopal Health Foundation, Health Reform Monitoring Survey – Texas, Issue Brief #3. Houston, Texas: 2014.
Download the full issue brief here.
The major provisions of the Affordable Care Act influencing health insurance coverage took effect this year. Residents of all 50 states who could not obtain affordable health insurance through their employer or in state insurance markets can now purchase coverage through the ACA’s Health Insurance Marketplace. Families earning between 100% and 400% of the federal poverty level are eligible for subsidies to purchase insurance in the Marketplaces. Individuals in families earning less than 138% of the federal poverty level are eligible for Medicaid if the state they live in elected the Medicaid expansion offered by the ACA. Under the law, almost all individuals are required to obtain health insurance coverage by March 31, 2014, or pay a penalty levied by the IRS in their tax return for 2014.
Given that Texas has consistently had the highest percent of uninsured residents among the 50 states for several years, the insurance provisions of the ACA are expected to play a substantial role in providing coverage to the close to 5 million adults who reportedly lacked health insurance in the state in 2010-2011. However, technical problems plagued the electronic websites for the Health Insurance Marketplaces in each state when they opened in October 2013, and some of these problems still exist today. In addition, Texas declined the Medicaid expansion offered by the ACA, so that most adults in families earning less than 138% of the federal poverty level are ineligible for any public subsidies to purchase health insurance.
In this brief, we track changes in health insurance status in Texas between September 2013 and March 2014. We find that the rate of uninsured adults ages 18 to 64 in Texas declined from 24.8% to 23.5%. The majority of this decline is attributable to an increase in the percent of adult Texans obtaining insurance through an employer. The proportions of adults with either Medicaid or individual private insurance both declined during this period. However, these percentages likely disguise significant changes in insurance coverage in Texas over the time period. By mid-March 2014, an estimated 746,000 Texans had obtained private insurance through the Marketplace. Of these, 225,000 (30.2%) were previously uninsured. Although a seemingly small proportion of Texans obtained insurance through the state’s Marketplace, the large absolute numbers had a substantial impact on increasing access to insurance coverage in the United States.
About the Survey
The Health Reform Monitoring Survey (HRMS) is a quarterly survey of adults ages 18-64 that began in 2013. It is designed to provide timely information on implementation issues under the ACA and changes in health insurance coverage and related health outcomes. HRMS provides quarterly data on health insurance coverage, access and use of health care, health care affordability, and self-reported health status. The Health Reform Monitoring Survey was developed by the Urban Institute, conducted by GfK and jointly funded by the Robert Wood Johnson Foundation, the Ford Foundation, and the Urban Institute. Rice University’s Baker Institute and The Episcopal Health Foundation are partnering to fund and report on key factors about Texans, obtained from an expanded, representative sample of Texas residents (HRMS-Texas). This Issue Brief is a summary of data extracted from the September 2013 and March 2014 rounds of the HRMS Survey in Texas. The Survey contains responses from 1,595 Texans in September 2013 and 1,538 in March 2014. We will continue to report on survey data through additional issue briefs and future surveys.
Insurance Status and Uninsured Rates for Adults Age 18–64
Figure 1 shows that from September 2013 to March 2014, Texas experienced an overall reduction in the rate of uninsured residents of 1.3 percentage points, from 24.8% to 23.5%, according to the March 2014 HRMS-Texas survey. This is similar to the national estimate of a 1.5% reduction reported by the Urban Institute for states that did not elect the ACA’s Medicaid expansion, as shown in Figure 2. This decline is substantially smaller than the 4 percentage point decrease in the percent uninsured in states that expanded Medicaid.
As Figure 1 shows, the decrease in the percent of uninsured Texans appears to be attributable to the increase in the share receiving insurance through an employer, which rose from 55.8% in September 2013 to 58.1% in March 2014. This increase in employer sponsored insurance is likely due to increased hiring by employers during this time period. Some of this increase may also be due to the ACA mandate for all individuals to purchase health insurance which may have caused employed people who had previously declined to participate in their employers’ plans to do so this year. Although the ACA requirement for larger employers to provide affordable health insurance does not become law until 2015, some employers may be offering lower cost options with limited provider networks to cover previously uninsured low-wage workers. The decrease in Texans covered by Medicaid is consistent with the state’s Medicaid enrollment data, which shows a decline in total enrollment over the same period of time. Most states, even those that did not expand Medicaid, experienced an increase in Medicaid enrollment which experts attribute to the increased public attention to health insurance because of the ACA. Due to a combination of logistical and systems changes, thousands of Texans lost or were delayed in being covered by Medicaid and/or CHIP between October 2013 and March 2014.
Figure 1 — Net Changes in Insurance Coverage Between September 2013 and March 2014, Texans Ages 18–64
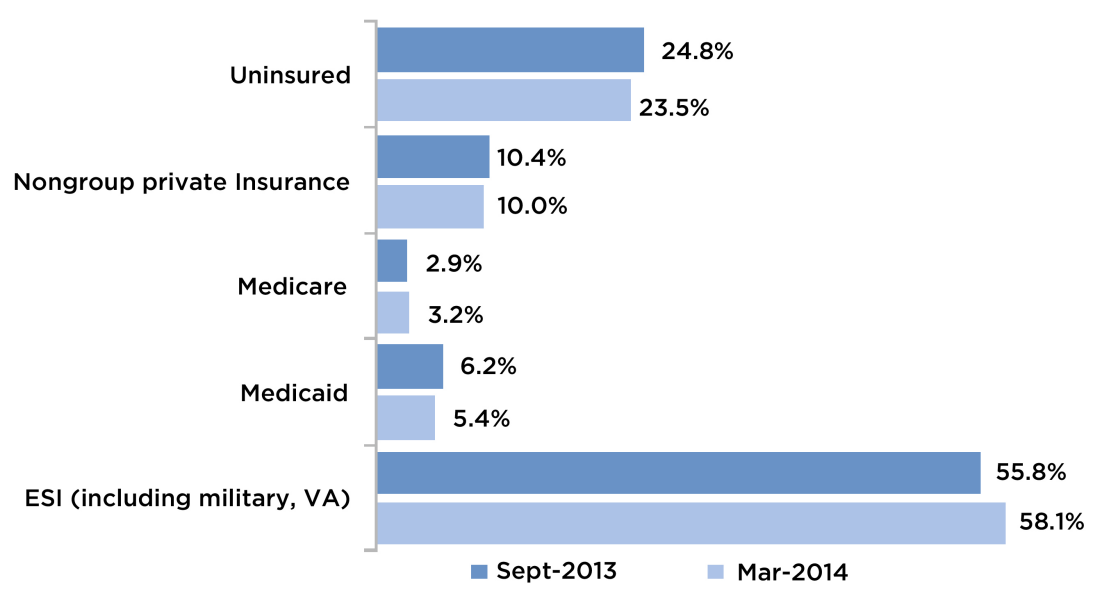
Figure 2 — Uninsured Rates for Adults Ages 18–64
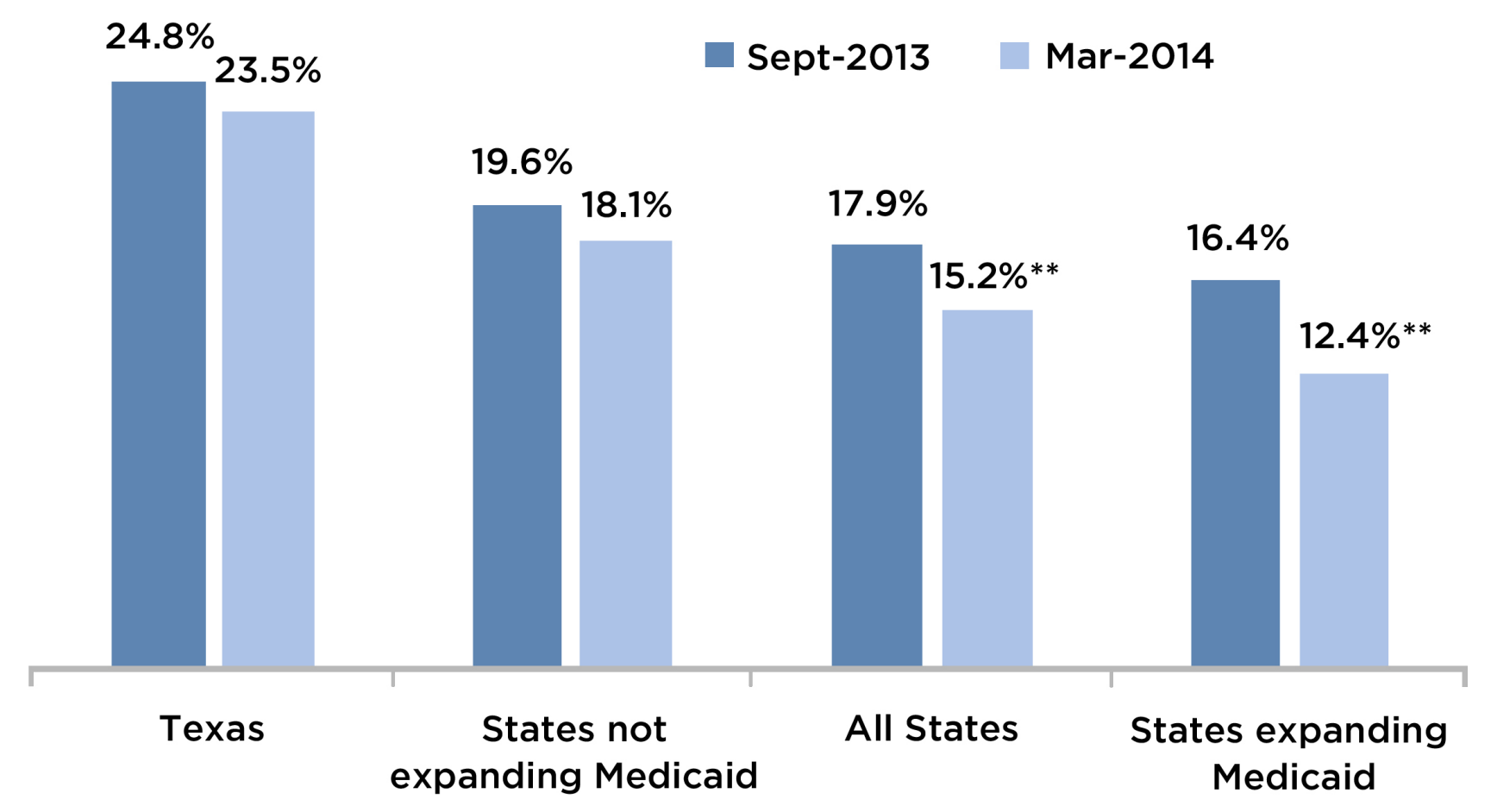
Notes “States expanding Medicaid” indicates those whose expansion took effect Before April 1, 2014. These are regression-adjusted estimates based on models that control for potential differences in the demographic, socioeconomic, and geographic characteristics of the HRMS sample across each quarter. */** Estimate differs significantly from the quarter 3 2013 uninsurance rate at the 0.05/0.01 levels, using two-tailed tests.
Figure 3 shows the changes in insurance status for Texans by income level based on the HRMSTexas March 2014 survey. The percent uninsured increased between September 2013 and March 2014 for the lowest income Texans, while those with highest incomes experienced the greatest decrease in uninsured rates. The increase in the lowest income group is consistent with the overall drop in Medicaid enrollment in Texas but is inconsistent with the experience of most other states, including those without Medicaid expansions, whose Medicaid rolls have increased over this time period.
Figure 3 — Percent Uninsured by Federal Poverty Level
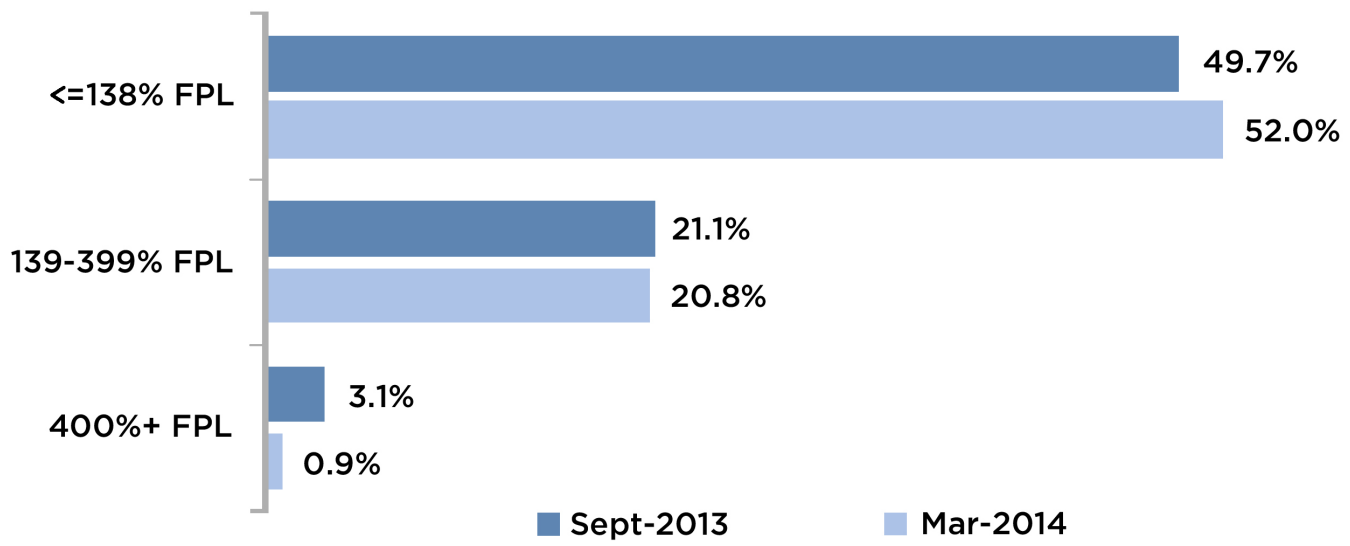
Texans and the Health Insurance Marketplace
A total of 4.6% of those surveyed in HRMS-Texas March 2014 responded yes to the question: “Did you enroll in a health insurance plan through the marketplace, also known as Healthcare.gov?” Applying this response rate to the adult population ages 18 to 64 in Texas equates to 746,000 Texans who enrolled in in a plan through the Marketplace by early March. This estimate is substantially higher than the US Department of Health and Human Services report that 295,025 Texans had enrolled as of March 1, 2014. However, national enrollment in Marketplace plans increased from 4.2 million on March 1 to 7.1 million on March 31st. The HRMS Texas survey was conducted throughout the month of March and likely captured a surge in enrollment before the March 31st deadline. Of those HRMS-Texas respondents who enrolled in a plan. 30.2% also indicated that they were without health insurance just prior to receiving coverage through the Marketplace. This response rate equates to 225,000 Texans who were newly covered with private health insurance through the Marketplace. We are unaware of any similar increase of this magnitude in private insurance coverage in Texas over a three month period.
Looking Ahead
In March 2014, the percent uninsured in Texas had declined only slightly, and the change appears to be attributable to increases in employer sponsored health insurance rather than the newly implemented Health Insurance Marketplace. The decline in uninsured is similar to that experienced by states that did not expand Medicaid under the ACA, and it falls far short of the 4 percentage point drop in uninsured experienced by states that elected to expand Medicaid. These percentage figures mask the impact of the Marketplace on the lives of hundreds of thousands of Texans. We will continue to track enrollment in the Texas Insurance Marketplace and rates of uninsured in Texas as the year progresses.
Methodology
Each quarter’s HRMS sample of nonelderly adults is drawn from active KnowledgePanel®members to be representative of the US population. In the first quarter of 2013, the HRMS provided an analysis sample of about 3,000 nonelderly (age 18–64) adults. After that, the HRMS sample was expanded to provide analysis samples of roughly 7,500 nonelderly adults, with oversamples added to better track low-income adults and adults in selected state groups based on (1) the potential for gains in insurance coverage in the state under the ACA (as estimated by the Urban Institute’s microsimulation model) and (2) states of specific interest to the HRMS funders.
Although fresh samples are drawn each quarter, the same individuals may be selected for different rounds of the survey. Because each panel member has a unique identifier, it is possible to control for the overlap in samples across quarters.
For surveys based on Internet panels, the overall response rate incorporates the survey completion rate as well as the rates of panel recruitment and panel participation over time. The American Association for Public Opinion Research (AAPOR) cumulative response rate for the HRMS is the product of the panel household recruitment rate, the panel household profile rate, and the HRMS completion rate—roughly 5 percent each quarter.
While low, this response rate does not necessarily imply inaccurate estimates; a survey with a low response rate can still be representative of the sample population, although the risk of nonresponse bias is, of course, higher.
All tabulations from the HRMS are based on weighted estimates. The HRMS weights reflect the probability of sample selection from the KnowledgePanel® and post-stratification to the characteristics of nonelderly adults and children in the United States based on benchmarks from the Current Population Survey and the Pew Hispanic Center Survey. Because the KnowledgePanel® collects in-depth information on panel members, the post-stratification weights can be based on a rich set of measures, including gender, age, race/ethnicity, education, household income, homeownership, Internet access, primary language (English/Spanish), residence in a metropolitan area, and region. Given the many potential sources of bias in survey data in general, and in data from Internet-based surveys in particular, the survey weights for the HRMS likely reduce, but do not eliminate, potential biases.


